Get Ready for the Winter Season: COVID-19, Flu, and RSV

With the world relaxing COVID-19 measures, countries removing travel restrictions, and people gathering indoors, experts are calling attention to the threat posed by COVID-19, influenza, and RSV this winter. In fact, SARS-CoV-2, influenza, and respiratory syncytial virus are already being reported to be co-circulating in many countries. Although the co-circulation of viruses is not uncommon, moderate surges and shifts in seasonal patterns observed with SARS-CoV-2, influenza, and RSV cases have caused significant concern regarding whether overlapping waves of these infections could overwhelm healthcare systems, cause capacity issues, disrupt service, or cause severe infections in people with lower immunity levels. Read along to learn more about the triple threat of COVID-19, influenza, and RSV.
Why should you be concerned about the convergence of COVID-19, influenza, and RSV?
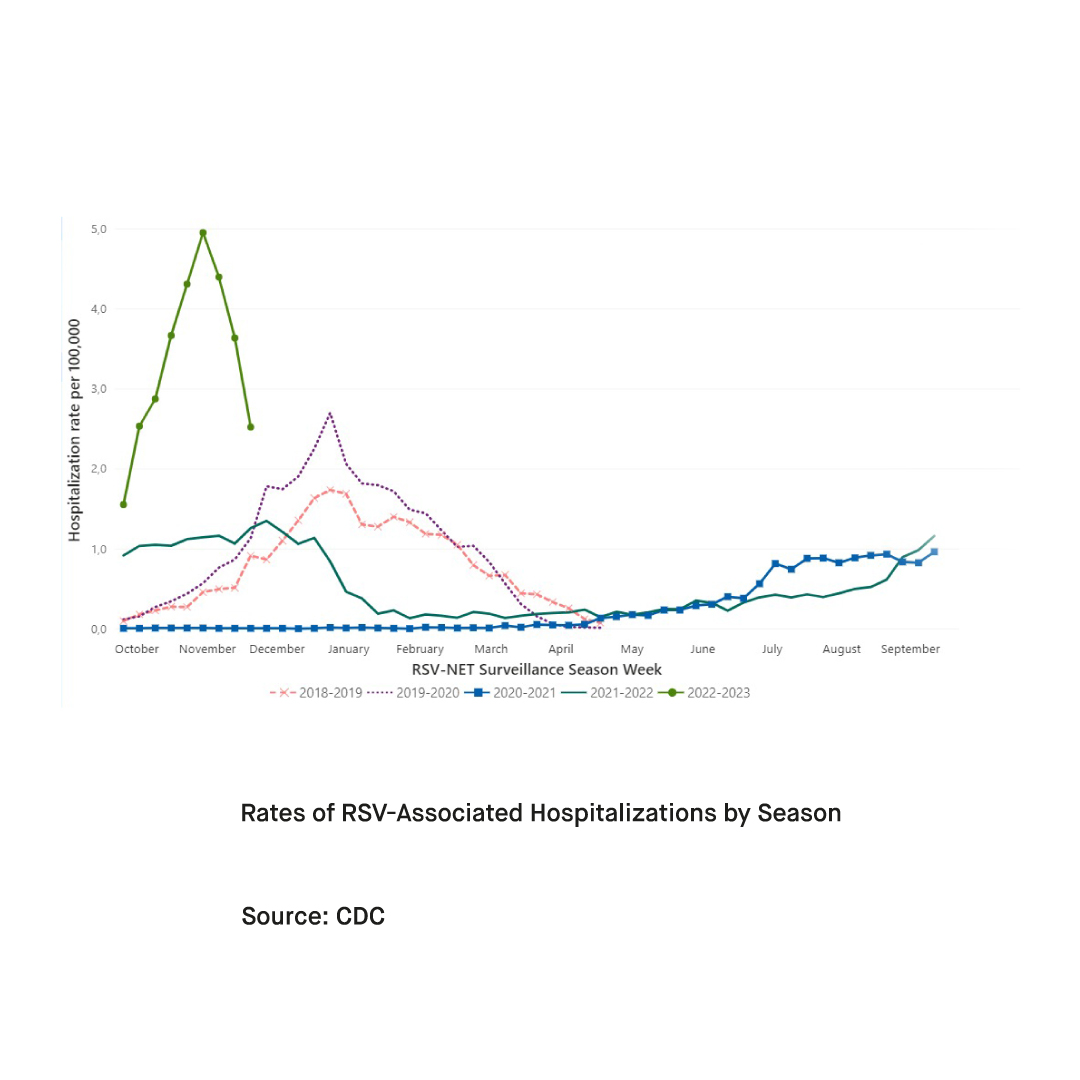
At the societal level, experts are concerned that if waves of COVID-19, influenza, and RSV peak around the same time, it could exhaust healthcare resources, supplies, and personnel. This exhaustion, in turn, could lead to delays and disruptions in care. Indeed, while respiratory viruses are known to circulate predominantly throughout the colder months, flu and RSV cases have appeared to be increasing earlier than usual this year. In many countries around the world, surges in influenza and RSV cases are already beginning to cause capacity issues in pediatric hospitals. Coupled with subsequent or overlapping waves of COVID-19, surges in influenza and RSV could overwhelm healthcare systems around the world.
In addition to the disruption of seasonal patterns, experts also highlight the impact of a potential immunity gap deriving from the pandemic measures taken over the past two years. Indeed, many adults and children are likely to have little or waning immunity against influenza and RSV following pandemic restrictions. Although RSV, influenza, and COVID-19 cause mild symptoms in most people, this immunity gap together with the rising rates of infection within the community, could put vulnerable groups at more risk of developing severe diseases. Older adults, children with low immunity, immunocompromised people, and those with certain health conditions may develop severe diseases, require hospitalization, and even die.
Who is at risk of developing the severe disease?

In general, older adults, newborn babies, young children, immunocompromised people, pregnant women, and those with multiple chronic medical conditions are the most vulnerable to severe disease and death caused by COVID-19, RSV, influenza, and other respiratory infections. Young children are especially susceptible to influenza and RSV. Moreover, those in direct contact with people at high risk should also be cautious of contracting these infections to prevent their transmission to vulnerable groups.
Is it possible to contract COVID-19, influenza, and RSV at the same time?
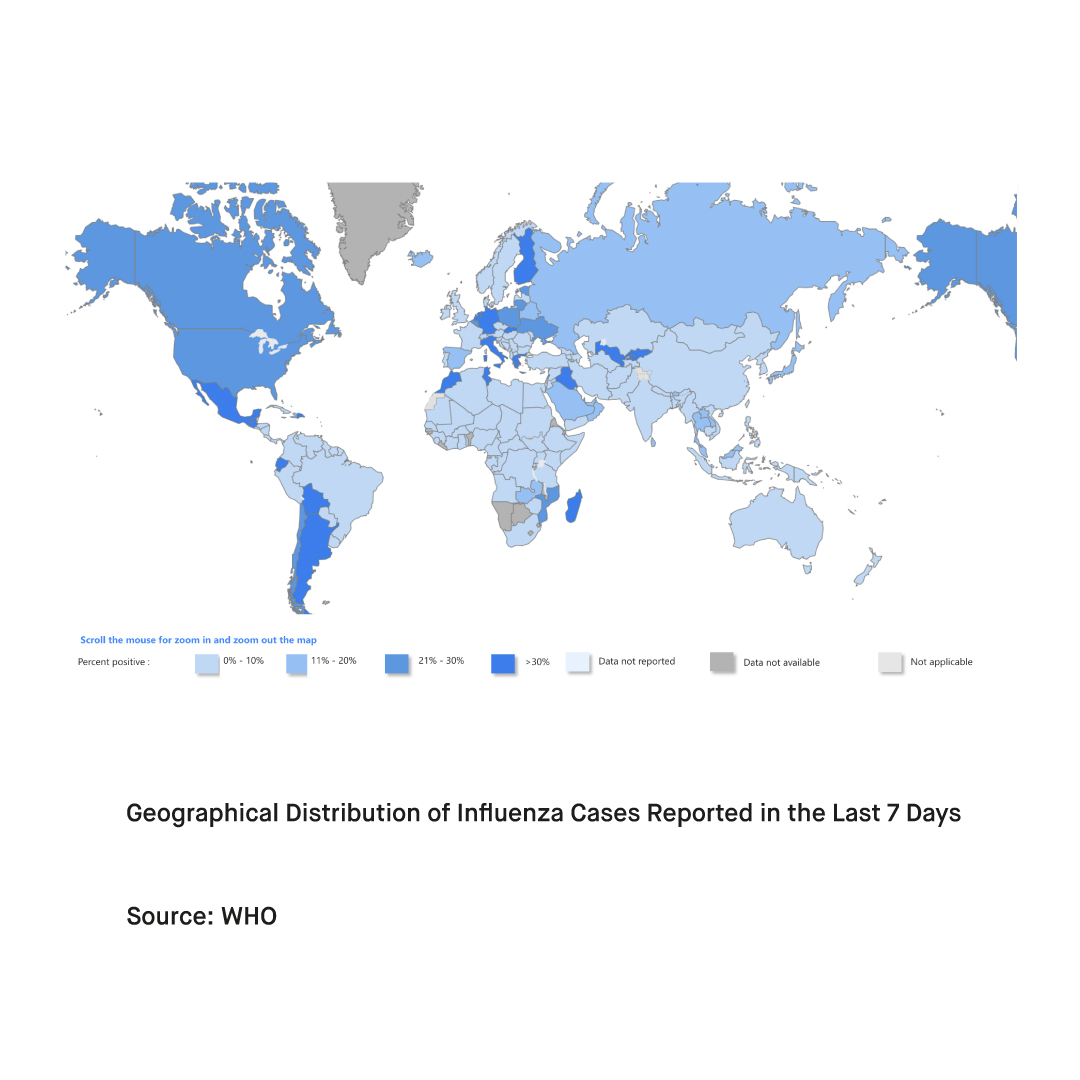
Despite their similar clinical presentations, SARS-CoV-2, RSV, and influenza are different viruses. Thus, it is theoretically possible to contract these viruses at the same time. However, people often do not contract all three viruses at once. Therefore, the main concern here derives from the simultaneous circulation of the three viruses rather than the occurrence of simultaneous infections with all three viruses.
How can you tell if you have COVID-19, influenza, or RSV?

There are some differences between the signs and symptoms associated with COVID-19 and influenza and RSV that could help you tell the virus you are most likely infected with. The initial symptoms of COVID-19 appear 2-14 days following exposure to SARS-CoV-2 and typically include fever, chills, cough, sore throat, runny/congested nose, loss of taste and smell, fatigue, myalgia, and headaches. Compared to COVID-19, influenza has a much more rapid onset. Appearing 1-2 days following infection, symptoms of influenza commonly include fever, chills, dry cough, sore throat, runny nose, myalgia, fatigue, and headache. In children, on the other hand, influenza often also causes gastrointestinal symptoms such as stomachache, nausea, vomiting, and diarrhea. Compared to COVID-19 and influenza, RSV often leads to milder infections with symptoms such as sneezing, runny nose, cough, fever, wheezing, and decreased appetite. Unfortunately, children infected with RSV can develop more serious infections. In fact, the Centers for Disease Control and Prevention (CDC) reports that RSV is the most common cause of lower respiratory tract infections in children younger than five years old.
However, it should be remembered that the slight differences between the clinical presentations of COVID-19, influenza, and RSV are often insufficient to differentiate these infections. Diagnostic testing is the most efficient and reliable strategy for the differential diagnosis of COVID-19, influenza, RSV, and other respiratory diseases with similar symptoms. Our RapidFor™ SARS-CoV-2 Rapid Antigen Test Kits, Influenza A/B Rapid Test Kit, and RSV Rapid Test Kits can detect these viruses in a variety of sample types and deliver highly accurate results in minutes. On the other hand, serological tests such as our RapidFor™ SARS-CoV-2 Rapid IgG/IgM Test Kit and RapidFor™ SARS-CoV-2 Neutralizing Antibody Test Kit help check for the level of vaccine-induced or infection-induced immunity against COVID-19. Last, our RapidFor™ SARS-CoV-2 & FLU A/B Antigen Combo Test Kit and SARS-CoV-2 + Flu A/B + RSV Combo Rapid Test Kit allow for the rapid simultaneous detection and differentiation of infections with COVID-19, influenza, and RSV.
What can you do to protect yourself against these infections?
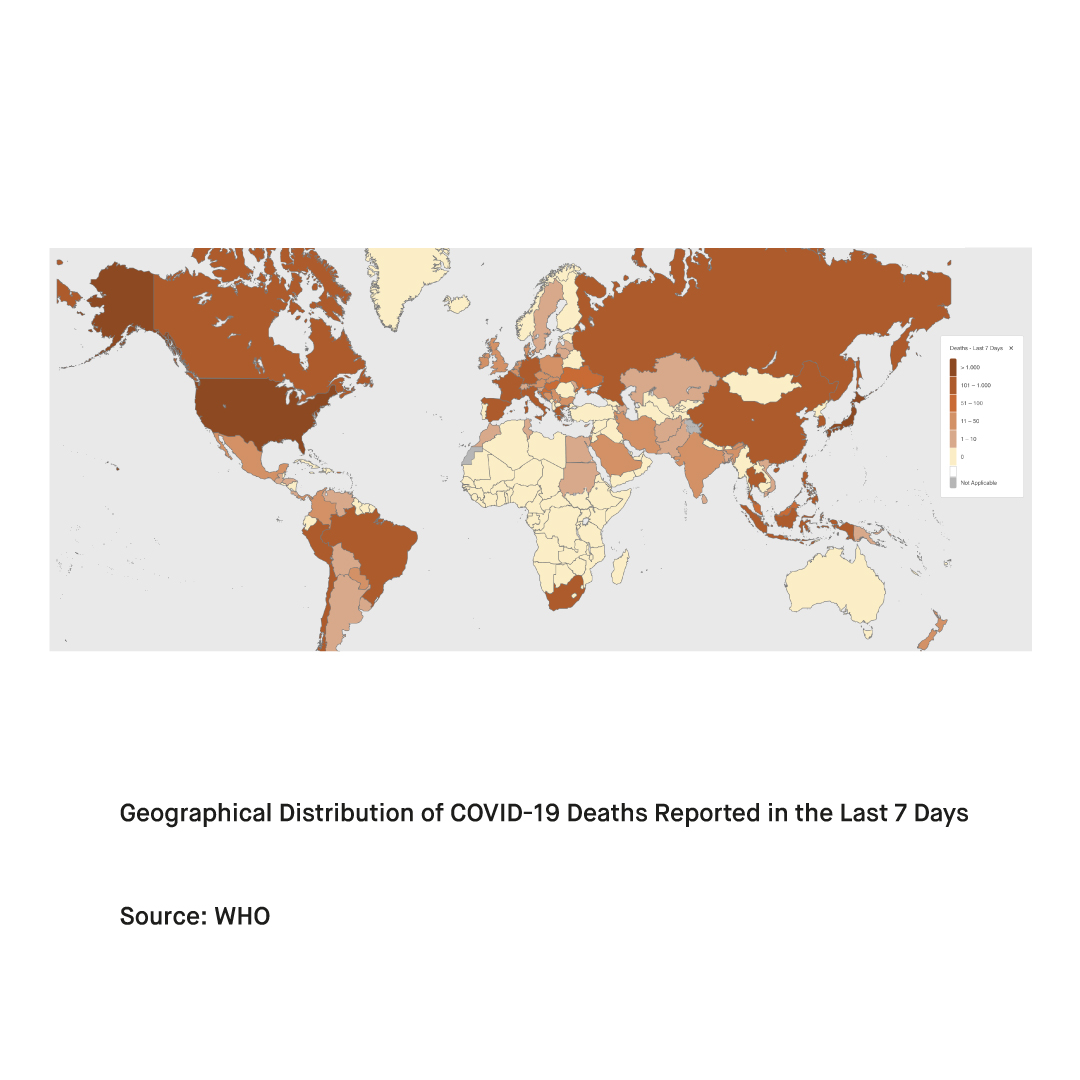
Vaccination is the most efficient strategy for the prevention of severe disease and complications associated with COVID-19 and influenza. Keeping up to date with vaccines and boosters is strongly advised to ensure the highest possible level of protection against severe disease from COVID-19. As for influenza, vaccines are updated each season according to the estimations of the dominant influenza subtype that will be in circulation. Influenza vaccines have proven to be particularly efficient during seasons where the estimations have overlapped with the subtype in circulation and thus have been recommended for those at risk of developing severe disease. Unfortunately, there is currently no vaccine available for RSV. Still, a monoclonal antibody preventative injection named palivizumab is available for use in children most susceptible to severe disease from infection with RSV.
Apart from vaccination, those who are at higher risk of developing severe disease, those with direct contact to vulnerable individuals, and those who want to reduce their risk of getting infected with SARS-CoV-2, influenza, and RSV can also continue to use masks, stick to personal hygiene rules, and try to avoid gatherings in indoor places.


