Sexually Transmitted Infections (STIs) are a pressing public health concern worldwide, affecting millions of people each year. Among the many STIs, one that often hides in the shadows, yet can have severe and long-lasting consequences if left untreated, is syphilis. In this blog, we will dive deep into the world of syphilis, exploring its causes, symptoms, diagnosis, treatment, and the importance of prevention.

Understanding Syphilis
Syphilis is a bacterial infection caused by the spirochete bacterium Treponema pallidum [1]. It primarily spreads through sexual contact, but it can also be transmitted from an infected mother to her unborn child during pregnancy [1]. The infection progresses in stages, each characterized by distinct symptoms and potential complications. There are four stages of syphilis: primary, secondary, latent, and tertiary syphilis [1-2].

Stages of Syphilis and Symptoms
- Primary Syphilis
- This stage begins with the appearance of a painless sore or ulcer known as a chancre at the site where the bacterium entered the body. Chancres are typically found on or around the genitals, anus, or mouth.
- The chancre usually heals on its own within a few weeks, even if left untreated.
- Secondary Syphilis
- If the infection is not treated during the primary stage, it progresses to the secondary stage. This stage is marked by a wide range of symptoms, including skin rashes, fever, sore throat, muscle aches, and swollen lymph nodes.
- These symptoms may come and go, but they can persist for weeks or even months.

- Latent Syphilis
- If the infection goes untreated even after the secondary stage, it enters the latent stage, where no symptoms are present. Latent syphilis can last for years, and the bacterium can still be present in the body.
- During this stage, the infection may remain asymptomatic or progress to the most severe form of syphilis, tertiary syphilis.

- Tertiary Syphilis
- Tertiary syphilis is the most serious and potentially life-threatening stage. It can damage various organs, including the heart, brain, nerves, eyes, and blood vessels.
- The complications from tertiary syphilis can be severe and irreversible, leading to disability and, in some cases, death.
Transmission of Syphilis
Syphilis is primarily transmitted through sexual contact, but it can also be transmitted from an infected mother to her unborn child during pregnancy. Here are the main modes of transmission for syphilis:
- Sexual Contact: Syphilis is most commonly spread through direct sexual contact with an infected person. This includes vaginal, anal, or oral sex [2]. The bacterium Treponema pallidum, which causes syphilis, can enter the body through mucous membranes and skin lesions, including chancres (sores) that are characteristic of primary syphilis [2].
- Mother-to-Child Transmission: Pregnant women with syphilis can transmit the infection to their unborn child through the placenta. This is known as congenital syphilis [3]. If not detected and treated early, congenital syphilis can result in serious health problems or even stillbirth [3].
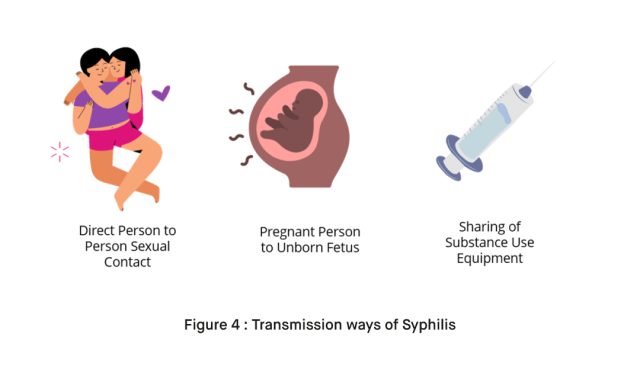
- Bloodborne Transmission: While syphilis is not as commonly transmitted through blood as some other STIs, it is theoretically possible. This may occur if a person with syphilis has an open sore or cut that comes into direct contact with the blood of another person, such as through sharing needles or syringes [2].
- Rare Non-Sexual Transmission: Although rare, syphilis can also be transmitted through non-sexual contact with an infected person, such as through close personal contact. This can occur when an individual comes into contact with a syphilis sore (chancre) or an open syphilis rash. However, this mode of transmission is not common.
It’s important to note that syphilis is highly contagious during the primary and secondary stages when chancres and other symptoms are present [3]. In later stages, when the infection becomes latent or progresses to tertiary syphilis, the risk of transmission to others decreases, but the potential for severe health complications remains.
To reduce the risk of syphilis transmission, it’s essential to practice safe sex by using latex or polyurethane condoms consistently and correctly, get regular STI screenings, and seek prompt medical treatment if you suspect you have syphilis or have been in close contact with an infected person. Early diagnosis and treatment are key to preventing the spread of syphilis and its associated health problems.
Epidemology of Syphilis
Syphilis is a global concern, with its impact varying by region and influenced by factors such as healthcare infrastructure, education access, and sexual behavior. Although it can affect individuals of all ages and genders, certain areas experience higher prevalence rates. Notably, young adults in their 20s and 30s are often at higher risk due to increased sexual activity and inconsistent protection use [4]. Men who have sex with men (MSM) face a heightened risk, witnessing significant increases in syphilis rates. However, the infection can affect people of any gender.
Annual infection rates fluctuate, with the United States reporting a notable increase in recent years. Meanwhile, Europe has seen an upward trend in syphilis incidence [4]. This regional variation underscores the importance of national and international monitoring and response [4]. Syphilis outbreaks can occur in specific communities linked to high-risk sexual behaviors and limited healthcare access, resulting in a sudden surge in cases.

Public health agencies respond by increasing education, testing, and treatment services in affected areas, aiming to reduce transmission and raise awareness. Understanding syphilis epidemiology is vital for developing effective prevention and control strategies, targeting high-risk groups, promoting education, and ensuring accessible testing and treatment, ultimately reducing its impact in various communities.
Prevention
Preventing syphilis is essential for protecting your sexual health and reducing the risk of this sexually transmitted infection (STI). Here are some key prevention measures [5]:
- Safe Sex Practices:
- Practice safe sex with consistent condom use, whether latex or polyurethane, to reduce the risk of syphilis and other STIs. Engage in sexual activities with a trusted partner, and both should undergo syphilis and STI testing before any sexual activity.
- Reducing the number of sexual partners can lower your risk of syphilis and other STIs. Limiting your sexual activity to a monogamous relationship with a partner who has also been tested for syphilis and other STIs can be an effective prevention strategy.
- Regular STI Testing:
- Get tested for syphilis and other STIs regularly, especially if you are sexually active or engage in high-risk sexual behaviors. Early diagnosis and treatment of syphilis are crucial to prevent its progression and complications.
- Avoid Sharing Needles:
- If you use drugs, do not share needles or syringes. Sharing injection equipment can lead to the transmission of syphilis and other bloodborne infections.

- Prenatal Care:
- If you are pregnant, seek early prenatal care and testing for syphilis. This is important to prevent the transmission of syphilis to your baby (congenital syphilis).
- Vaccination:
- While there is no vaccine for syphilis, getting vaccinated against other preventable STIs, such as hepatitis B and human papillomavirus (HPV), can reduce your overall risk of STIs.
- Seek Treatment Early:
- If you are diagnosed with syphilis, it’s important to follow your healthcare provider’s treatment recommendations. Early treatment with antibiotics, typically penicillin, is highly effective in curing syphilis.
Treatment of Syphilis
The treatment for syphilis differs depending on its stage. In the early stages, such as primary and secondary syphilis, a single injection of a long-acting penicillin is the preferred course of action [2]. For those with a penicillin allergy, alternative antibiotics like doxycycline or tetracycline are available, although penicillin remains the top choice [6].
When it comes to latent syphilis, the treatment approach depends on whether it’s in its early or late stage. If it’s early latent syphilis (less than a year in duration), a single dose of benzathine penicillin G typically does the trick [6]. Late latent syphilis, lasting more than a year, may necessitate three weekly doses of benzathine penicillin G to ensure complete eradication of the infection.
For tertiary syphilis, which involves severe complications, a more extensive treatment plan is required, often including intravenous penicillin G [6].
When syphilis affects the nervous system, a condition known as neurosyphilis, the treatment typically involves a more intensive regimen, with intravenous penicillin G administered daily for 10 to 14 days [6].
If you suspect you have syphilis or have been exposed to the infection, seeking prompt medical attention is essential. Early diagnosis and treatment are paramount in halting the progression of syphilis and averting the development of severe complications.
Diagnosis Methods
Certainly, in addition to the traditional laboratory-based blood tests, rapid test kits have become increasingly available for the diagnosis of syphilis. Here’s an updated overview of the diagnostic methods for syphilis, including the use of rapid test kits:
- Clinical Evaluation:
- A healthcare provider begins the diagnostic process by taking a comprehensive medical history and conducting a physical examination. They inquire about any signs and symptoms and assess potential risk factors.
- Blood Tests:
- Blood tests are the most common and reliable way to diagnose syphilis. There are two types of blood tests used:
- Non-Treponemal Tests: These tests, like the Rapid Plasma Reagin (RPR) and Venereal Disease Research Laboratory (VDRL) tests, detect antibodies in response to the infection and may be used as initial screening tests [7].
- Treponemal Tests: Treponemal tests, such as the Fluorescent Treponemal Antibody Absorption (FTA-ABS) and Treponema Pallidum Particle Agglutination (TP-PA) tests, confirm syphilis diagnosis after a positive non-Treponemal test result [7]. These tests detect antibodies specific to the syphilis bacterium and remain positive even after successful treatment.
- Blood tests are the most common and reliable way to diagnose syphilis. There are two types of blood tests used:
- Cerebrospinal Fluid Analysis:
- If neurosyphilis is suspected, a lumbar puncture (spinal tap) may be performed to analyze cerebrospinal fluid for signs of infection.
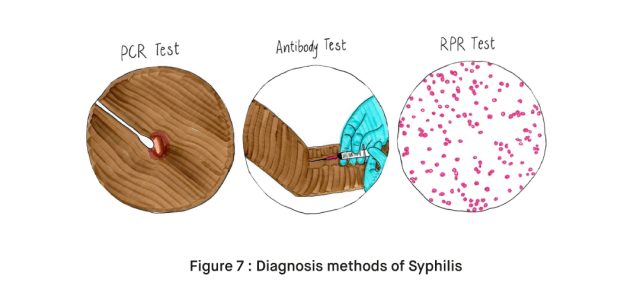
- Direct Visualization:
- In cases where syphilis sores (chancres) are present, a healthcare provider may perform a dark-field microscopy examination of material from the sore to identify the spirochete bacterium Treponema pallidum.
- Swab Tests:
- For oral or genital lesions, swab samples may be collected for polymerase chain reaction (PCR) testing, which detects the presence of the bacterium’s genetic material.
- Rapid Test Kits:
- Rapid test kits are becoming more accessible for syphilis diagnosis. These kits are point-of-care tests that provide quick results, often within minutes. They are particularly useful in settings where timely diagnosis and treatment are crucial, such as in resource-limited areas or during outreach programs.
- Screening During Pregnancy:
- Pregnant women are often screened for syphilis as part of their prenatal care. Screening is essential to prevent the transmission of syphilis to the unborn child (congenital syphilis).
The choice of diagnostic method may depend on factors such as the availability of resources and the specific healthcare setting. Regardless of the method used, accurate and timely diagnosis of syphilis is essential for initiating appropriate treatment and preventing the progression of the infection and its complications. If you suspect you have syphilis or have been exposed to the infection, it’s important to seek medical attention promptly for testing and diagnosis.
How to Use Syphilis (Treponema Pallidum) Rapid Test Kit?
Using a syphilis (Treponema pallidum) rapid test kit typically involves a few simple steps. These rapid test kits are designed for quick, point-of-care syphilis testing and can be used by healthcare professionals or trained individuals. It’s important to follow the manufacturer’s instructions provided with the specific kit you are using, as the exact steps may vary slightly. However, here is a general guide on how to use a syphilis rapid test kit:
Materials Needed:
- Syphilis rapid test kit (provided by the manufacturer)
- Safety gloves (recommended)
- A clean and flat surface for performing the test
- Timer or stopwatch (for timing the test)
Steps to Use a Syphilis Rapid Test Kit:
- Read the Instructions: Start by carefully reading the instructions provided with the kit. The instructions will include important information on the correct procedure, required materials, and interpretation of results. Follow the instructions precisely.
- Gather Supplies: Ensure that you have all the necessary materials ready, including the test kit, safety gloves, and a clean, flat surface to work on.
- Prepare the Test Kit: Remove the test kit from its packaging and check for any visible damage. Ensure that it is within the expiration date. The kit typically consists of a test device, a sample collection swab or lancet, reagents, and a buffer solution.
- Prepare the Sample: Depending on the specific kit, you may need to collect a blood sample, serum, or plasma. Follow the instructions to collect the sample using the provided swab or lancet. Be sure to follow all safety precautions and proper hygiene during sample collection.
- Apply the Sample to the Test Device: Apply the collected sample to the designated area on the test device, following the instructions carefully. This may involve placing a drop of the sample onto the test device.
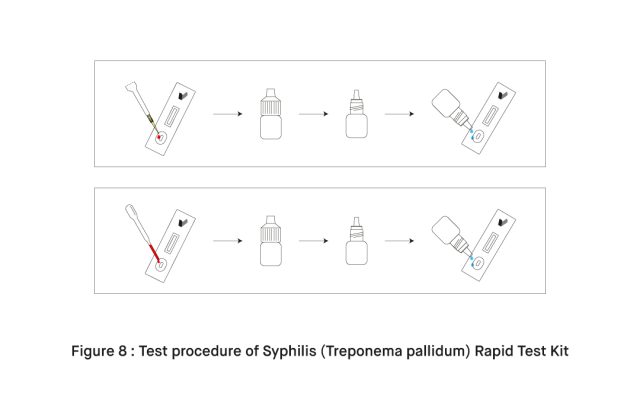
Test procedure of Syphilis (Treponema pallidum) Rapid Test Kit - Add Buffer Solution: Add the buffer solution provided in the kit to the test device. This solution helps the test react and provides accurate results.
- Wait for Results: Follow the recommended waiting time (specified in the instructions) for the test results to develop. Typically, you will need to wait for a specific duration, such as 10-15 minutes.
- Read and Interpret Results: After the designated waiting time, check the test device for the appearance of lines or other indicators, as per the manufacturer’s instructions. A positive or negative result will be indicated by the presence or absence of specific lines or symbols on the test device. It’s important to follow the interpretation guidelines provided in the instructions.
- Dispose of Materials: Safely dispose of any used materials, including the sample collection swab or lancet, according to proper biohazard disposal procedures.
- Document the Results: Record the results of the test as either positive or negative. Accurate record-keeping is essential for healthcare documentation.
Remember that the interpretation of rapid test results should be done by a trained healthcare professional. If a syphilis test is positive, it is essential to seek further evaluation and confirmatory testing by a healthcare provider for diagnosis and treatment. False-positive or false-negative results can occur, so confirmatory tests are typically necessary to ensure accuracy.
The Most Effective and Commonly Used Syphilis Rapid Test Kit
The Anti-Syphilis Rapid Test Kit is a user-friendly, point-of-care tool designed for qualitative syphilis screening in human serum, plasma, and whole blood samples. Its advantages include early detection and immediate treatment initiation, which is vital for preventing transmission and reducing the overall prevalence of syphilis. The test also helps prevent long-term complications associated with the disease and unfavorable pregnancy outcomes. Its easy sampling and simple procedure make it accessible, and the results are easily interpretable, making it a valuable tool for both healthcare professionals and individuals seeking self-testing options, ultimately contributing to improved syphilis control and public health.
REFERENCES
[1] Syphilis — CDC detailed fact sheet. Centers for Disease Control and Prevention. https://www.cdc.gov/std/syphilis/stdfact-syphilis-detailed.htm. Accessed November 9, 2023.
[2] Sexually transmitted infections treatment guidelines, 2021: Syphilis. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/syphilis.htm. Accessed November 9, 2023
[3] Garnett, G. P., Aral, S. O., Hoyle, D. V., WILLARD CATES, J., & Anderson, R. M. (1997). The natural history of syphilis: implications for the transmission dynamics and control of infection. Sexually transmitted diseases, 24(4), 185-200.
[4] Syphilis – Annual Epidemiological Report 2021. European Centre for Disease Prevention and Control. (2023b, October 23). https://www.ecdc.europa.eu/en/publications-data/syphilis-annual-epidemiological-report-2021
[5] Saloojee, H., Velaphi, S., Goga, Y., Afadapa, N., Steen, R., & Lincetto, O. (2004). The prevention and management of congenital syphilis: an overview and recommendations. Bulletin of the World Health Organization, 82(6), 424-430.
[6] Clement, M. E., Okeke, N. L., & Hicks, C. B. (2014). Treatment of syphilis: a systematic review. Jama, 312(18), 1905-1917.
[7] Larsen, S. A., Steiner, B. M., & Rudolph, A. H. (1995). Laboratory diagnosis and interpretation of tests for syphilis. Clinical microbiology reviews, 8(1), 1-21.


