What is the Human Papillomavirus (HPV) and How Does the Human Papillomavirus (HPV) Test Kit Work?

Promoting uncontrollable cell generation and transformation in the host body, oncogenic viruses account for around 12% of all human cancers worldwide. Among oncogenic viruses, human papillomaviruses (HPV) have a prominent position due to their significant role in developing cervical and other cancers. Today, despite the recent advances in our understanding of human papillomaviruses’ biology, pathology, and vaccinology (HPV), the number of cancers associated with the infection continues to grow worldwide.
What is Human Papillomavirus (HPV)?
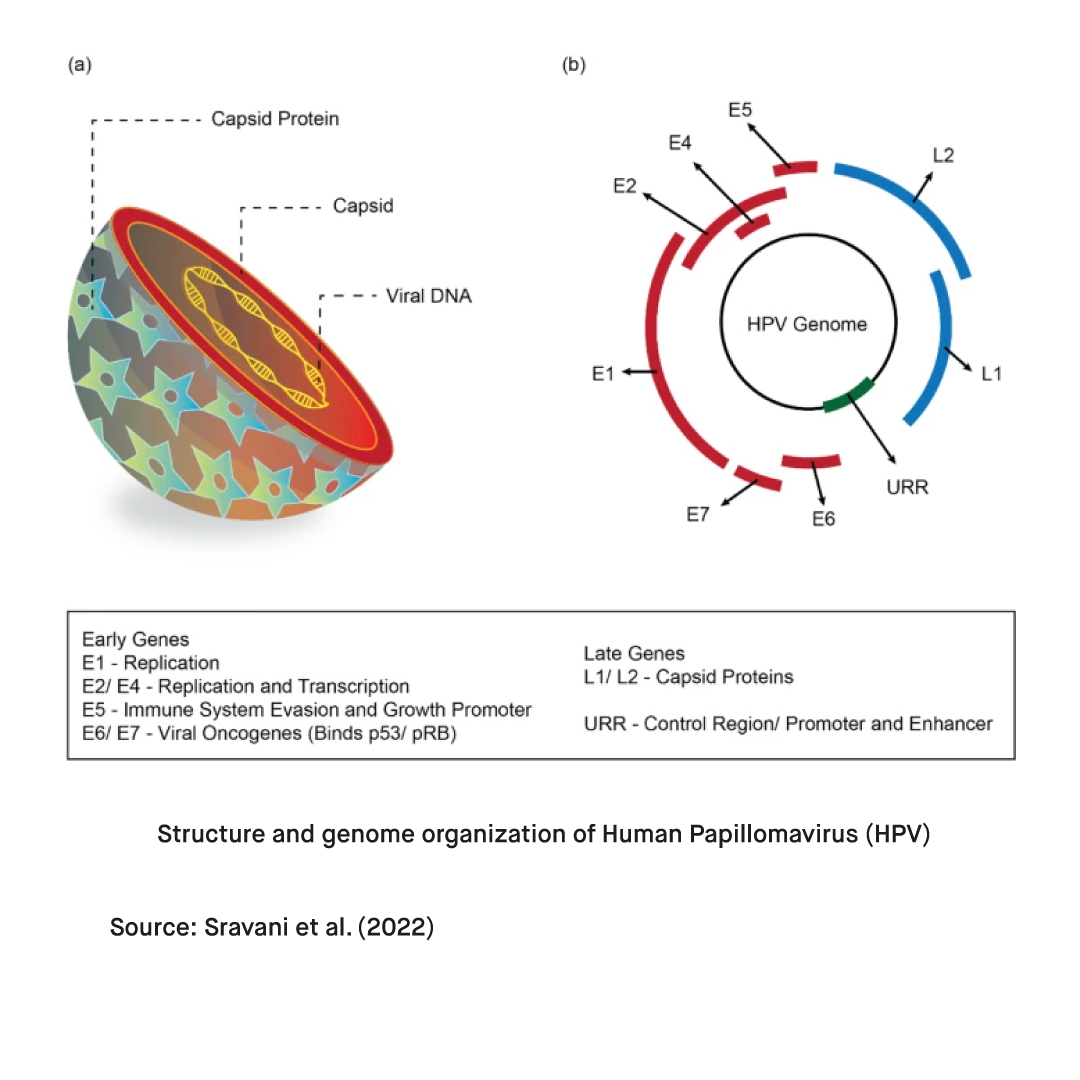
Papillomaviruses are a large group of non-enveloped double-stranded DNA viruses that belong to the papillomavirus genus of the Papillomaviridae family. Human papillomaviruses (HPV) can infect epithelial cells of the skin as well as oral and genital mucosa. Human papillomaviruses (HPV) spreads through intimate skin-to-skin contact, including vaginal, anal, or oral sex. More than 100 types of human papillomavirus (HPV) have been detected so far, which have been further categorized as cutaneous or mucosal depending on their tissue tropism and as high risk (HR) or low risk (LR) depending on their oncogenic capacity. Human papillomavirus (HPV) is currently among the most common sexually transmitted infections worldwide. According to the Centers for Disease Control and Prevention (CDC), around 13 million new cases of HPV are detected each year. In fact, it is estimated that around 80 percent of sexually active men and women get infected with HPV at some point in their lives (Perez-Campos Mayoral et al., 2018).
What are the symptoms of infection with Human Papillomavirus (HPV)?

Although they can still transmit the infection, some people infected with human papillomavirus (HPV) may not exhibit any signs or symptoms. Symptomatic cases of HPV commonly present with warts that may develop in the vagina, vulva, urethra, penis, anus, or throat. These warts may be more or less visible, appear as raised or flat, and come in different sizes. Although these warts usually do not cause any additional symptoms, some people may occasionally experience burning pain, itching, or discomfort in the affected area.
How concerned should you be about getting infected with Human Papillomavirus (HPV)?

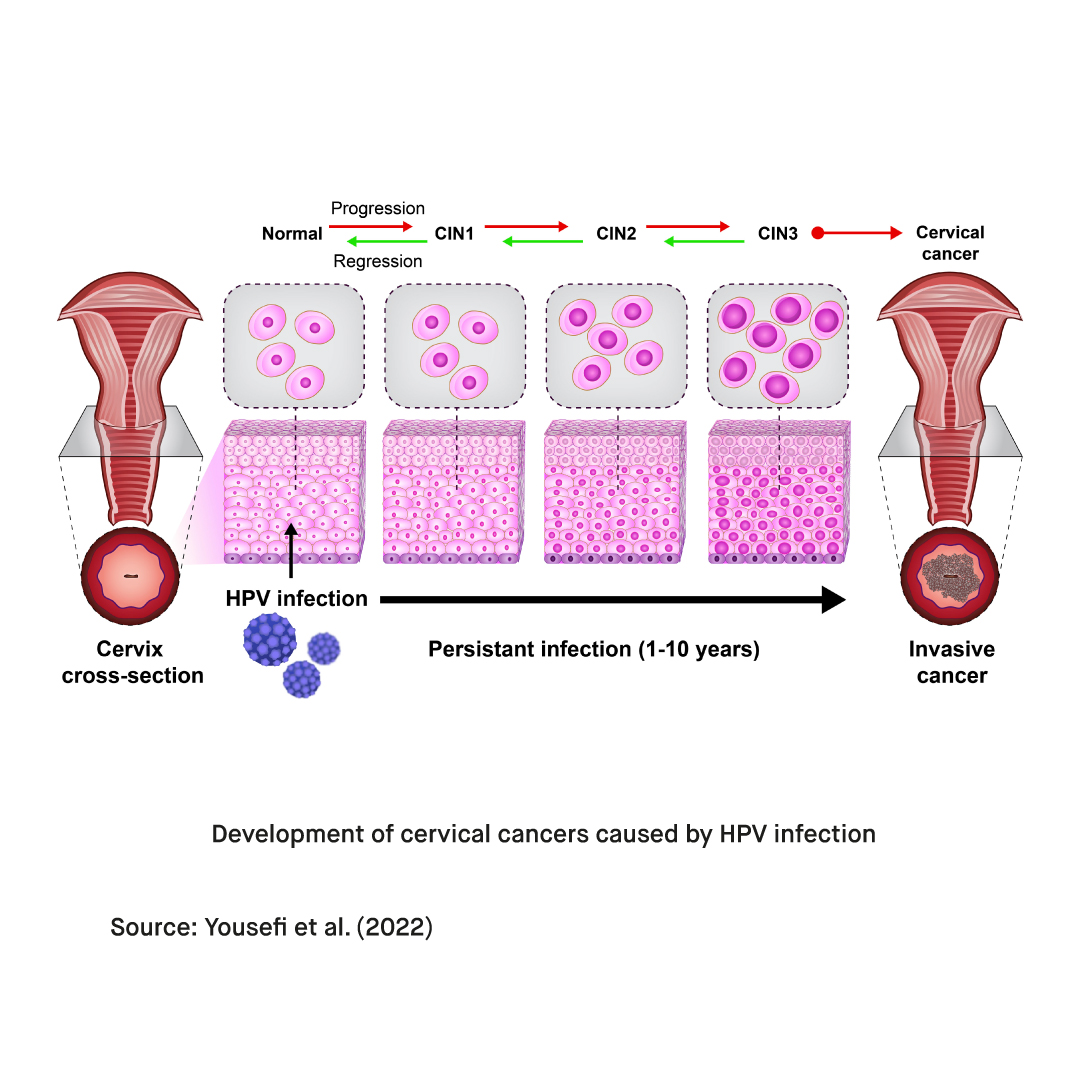
Most infections with human papillomavirus (HPV) go away within 1 to 2 years. However, persistent infections with certain types of human papillomavirus (HPV) are associated with various forms of pre-malignant and malignant lesions such as cervical, anogenital, esophageal, and breast carcinomas as well as carcinomas in the head and neck. In fact, according to de Sanjosé et al. (2018), human papillomavirus (HPV) is currently known to account for approximately 5% of all cancers and 30% of all infectious agent-related cancers worldwide. It is also among the most common causes of cervical cancer in women. Currently, cervical cancer is the third most common malignancy and the fourth most common cause of death in women worldwide.
How can you get tested for Human Papillomavirus (HPV)?
Alongside visual examination of symptoms, biopsies, and Pap smear tests, the diagnosis of infections with human papillomavirus (HPV) may involve the use of molecular tests based on DNA detection and serological tests. Since the integration of the viral DNA into the host cell chromosomes may lead to deletions or rearrangements at the E1/E2 region of the viral genome during tumor development, nucleic acid detection methods intended for the detection of HPV target the L1, upstream regulatory region (URR) or the E6/E7 genes in the infected cells. SerOn the other hand, serological tests get antibodies against human papillomavirus (HPV) as a marker of prior infection with the virus. Utilizing HPV-specific antigens, these tests can be used to both examine the epidemiology of human papillomavirus (HPV) and check the immunogenicity of vaccines.
How can you protect yourself against Human Papillomavirus (HPV)?

Vaccination is the most efficient strategy to protect yourself against infections with human papillomavirus (HPV). Most viral vaccines and prophylactic vaccines for human papillomavirus (HPV) have been demonstrated to induce substantial immune responses against persistent infections and premalignant neoplasia. By activating humoral immunity, triggering the production of virus-neutralizing antibodies, and preventing the entry of viruses to host cells, prophylactic vaccines have proved to offer efficient protection against HPV. Prophylactic vaccines have been created by recombinant DNA technology utilizing the HPV L1 capsid proteins of the virus and noninfectious virus-like particles (VLPs). As of now, Gardasil, Cervarix, and Gardasil-9 are the three prophylactic vaccines licensed for use against infections with high-risk HPV. Therapeutic vaccines, on the other hand, function by stimulating cell-mediated immunity instead of neutralizing antibodies. There are currently no therapeutic vaccines that are approved for use in infection with human papillomavirus (HPV). However, efforts for the development of a safe and efficient therapeutic vaccine against the virus are underway.
In addition to vaccination, refraining from unsafe sexual practices such as having unprotected oral, anal, or vaginal intercourse, frequently changing sexual partners, and intimate contact with potentially infected people can help reduce the risk of getting infected with human papillomavirus (HPV). Finally, getting informed on the common symptoms of the infection, prompt diagnosis, timely treatment, and effective contact tracing can prevent the further transmission of the virus.
REFERENCES
De Sanjosé, S., Brotons, M., & Pavón, M. A. (2018). The natural history of human papillomavirus infection. Best Practice &Amp; Research Clinical Obstetrics &Amp; Gynaecology, 47, 2–13. https://doi.org/10.1016/j.bpobgyn.2017.08.015
Parrott, G. L., Kinjo, T., & Fujita, J. (2016). A Compendium for Mycoplasma pneumoniae. Frontiers in Microbiology, 7. https://doi.org/10.3389/fmicb.2016.00513
Perez-Campos Mayoral, E., Mayoral-Andrade, G., Pérez-Campos Mayoral, L., Canseco, S. P., Cruz, R. M., Hernández-Huerta, M. T., Rodriguez, A. M., Cabrera-Fuentes, H. A., & Pérez-Campos, E. (2018). Diagnosis of Transient/Latent HPV Infections – A Point of View! Archives of Medical Research, 49(5), 293–296. https://doi.org/10.1016/j.arcmed.2018.10.004
Sravani, A. B., Ghate, V., & Lewis, S. (2022). Human papillomavirus infection, cervical cancer and the less explored role of trace elements. Biological Trace Element Research. https://doi.org/10.1007/s12011-022-03226-2
Yousefi, Z., Aria, H., Ghaedrahmati, F., Bakhtiari, T., Azizi, M., Bastan, R., Hosseini, R., & Eskandari, N. (2022). An Update on Human Papilloma Virus Vaccines: History, Types, Protection, and Efficacy. Frontiers in Immunology, 12. https://doi.org/10.3389/fimmu.2021.805695


