Human Papillomavirus (HPV) is a prevalent and potentially dangerous infection that affects millions of people worldwide. This tiny, DNA-containing virus is known for its association with cervical cancer, making it a significant health concern for individuals of all ages. In this blog, we will delve into the world of HPV, exploring its various aspects, transmission, the critical role it plays in the development of cervical cancer and HPV diagnostic test kits, such as HPV Rapid Test Kit and HPV PCR Detection Kit.

Understanding HPV
HPV is a group of related viruses, with more than 200 different types identified. While most HPV infections resolve on their own without causing any health problems, certain high-risk types can lead to serious conditions, including cervical cancer. The virus is primarily transmitted through intimate skin-to-skin contact, often during sexual activity. It can affect various parts of the body, including the genital area, mouth, and throat.
Causes of HPV
The primary cause of HPV is the transmission of the virus through direct contact with an infected person’s skin or mucous membranes. Sexual activity, including vaginal, anal, or oral sex, is the most common mode of transmission. Moreover, the virus can be spread even when an infected individual does not display any visible symptoms. Certain lifestyle factors, such as smoking and a weakened immune system, may increase the risk of persistent HPV infection.
Symptoms of HPV
In many cases, HPV infections do not manifest any noticeable symptoms, making it challenging for individuals to know if they are infected. However, some HPV types can cause visible warts on the genitalia or surrounding areas. High-risk HPV types, especially types 16 and 18, may lead to abnormal cell changes in the cervix, potentially progressing to cervical cancer over time.

Additionally, HPV can cause 6 different types of cancers. These are cervical cancer, cervical precancer, oropharyngeal cancer, anal cancer, vulvar and vagina cancer and penile cancer.

Risk Groups
Certain groups of individuals face a higher risk of HPV infection and its associated complications. Adolescents and young adults are particularly susceptible due to increased sexual activity. Immunocompromised individuals, such as those living with HIV/AIDS, also face an elevated risk. Additionally, smokers and individuals with a weakened immune system are more prone to persistent HPV infections.
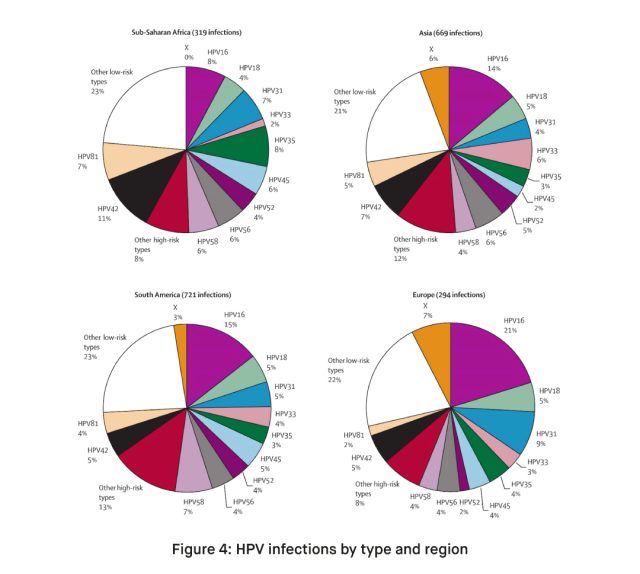
Epidemiology of HPV
HPV is one of the most common sexually transmitted infections globally. According to epidemiological studies, the majority of sexually active individuals will contract at least one type of HPV during their lifetime. The prevalence of the virus varies across different populations and age groups. Vaccination campaigns aim to reduce the burden of HPV-related diseases worldwide.

Prevention Methods
Vaccination against HPV is a powerful preventive measure, effectively guarding against the most common high-risk strains. Safe sexual practices, including consistent condom use, also contribute to reducing the risk of transmission. Education and awareness campaigns play a pivotal role in promoting preventive measures.

Diagnosis Methods and Treatments
Various diagnostic methods, including Pap tests, HPV tests, and colposcopy, test kits are employed to detect and evaluate HPV infections and related changes in the cervix. Early diagnosis is essential for successful treatment and management of HPV-related cervical abnormalities. Treatments may include surgery, radiation therapy, and chemotherapy, depending on the severity and stage of cervical cancer.
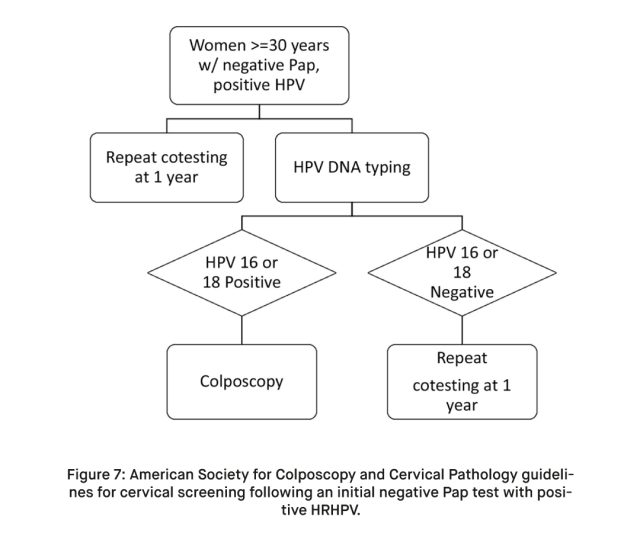
It’s important to note that routine screenings and early detection are key in managing HPV infections, as they can help prevent the development of cervical cancer. Individuals should discuss the most appropriate screening methods and frequency with their healthcare providers based on their age, risk factors, and overall health.
How to Use Human Papilloma Virus (HPV) Rapid Test Kit and PCR Detection Kit?
Using a Human Papillomavirus (HPV) Rapid Test Kit and PCR Detection Kit typically involves a series of steps to ensure accurate and reliable results. Below are general guidelines for using these types of kits. However, it’s crucial to follow the specific instructions provided by the manufacturer of the kit you are using, as protocols may vary.
HPV Rapid Test Kit:
- Read the Instructions:
- Carefully read and understand the manufacturer’s instructions provided with the HPV Rapid Test Kit.
- Sample Collection:
- Collect the appropriate sample, which may be swabs from the affected area, such as the cervix, vagina, or oral cavity, depending on the type of test.
- Prepare the Test Device:
- Open the test kit and remove the test device.
- Ensure that the test device is within its expiration date.
- Apply the Sample:
- Apply the collected sample to the designated area on the test device as per the instructions.

- Wait for Results:
- Allow the test to run for the specified time.
- Observe the appearance of lines or other indicators to interpret the results.
- Results are usually visible within a specific timeframe, typically within minutes.
- Interpret Results:
- Follow the kit instructions for interpreting the test results.
- Results may include positive, negative, or invalid outcomes.
HPV PCR Detection Kit:
- Read the Instructions:
- Carefully read and understand the manufacturer’s instructions provided with the HPV PCR Detection Kit.
- Sample Collection:
- Collect the appropriate sample, typically DNA extracted from cells in the affected area.
- Prepare PCR Reaction Mix:
- Follow the kit instructions to prepare the PCR reaction mix, including primers, probes, and other necessary components.
- Load Samples:
- Add the extracted DNA samples to the PCR reaction mix.

- Run PCR Reaction:
- Use a PCR machine to run the amplification reaction according to the kit’s cycling parameters.
- Analysis of PCR Products:
- Analyze the PCR products using gel electrophoresis or another appropriate method, following the kit instructions.
- Interpret Results:
- Interpret the results based on the presence or absence of specific DNA bands corresponding to the targeted HPV genotypes.
Always adhere to good laboratory practices and follow the manufacturer’s guidelines precisely. If you are not familiar with molecular biology techniques, consider seeking assistance from a qualified laboratory professional. Additionally, consult with healthcare providers for appropriate sample collection and result interpretation.
The Most Effective and Commonly Used Rapid Test Kits for Human Papilloma Virus (HPV)
The HPV Rapid Test Kit is an innovative in vitro diagnostic solution designed for the rapid and qualitative detection of human papillomavirus (HPV) nucleic acids. Utilizing a quick and straightforward testing process, this kit allows for the efficient assessment of HPV presence in various samples, such as skin, oral, and anogenital specimens. With its user-friendly design, the HPV Rapid Test Kit provides a valuable resource for healthcare professionals, offering prompt results that aid in the early identification of HPV infections. This rapid and reliable testing solution plays a crucial role in proactive healthcare strategies, contributing to timely interventions and informed management of HPV-related conditions.
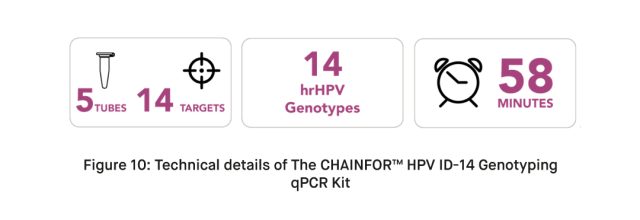
The CHAINFOR™ HPV ID-14 Genotyping qPCR Kit is a highly precise diagnostic tool utilizing real-time PCR technology for the qualitative detection of 14 high-risk HPV genotypes, including those linked to cancer development. Engineered with precision, the kit offers a comprehensive means of identifying these genotypes in genomic DNA specimens. Targeting high-risk genotypes, such as 16, 18, 31, and others, associated with cancer, it serves as a valuable resource for healthcare professionals, enabling efficient and accurate detection of HPV DNA. The cutting-edge qPCR technology empowers early intervention and management of HPV-related conditions, playing a crucial role in proactive strategies for preventing and managing HPV-associated cancers.
The CHAINFOR™ HPV Screening ID-15 qPCR Kit is an advanced in vitro diagnostic solution designed for precise detection of 15 high-risk HPV genotypes using real-time PCR technology. Meticulously crafted to identify specific genotypes, including 16, 18, and 51, this screening tool provides accurate information for early identification of HPV types associated with health risks. The sophisticated qPCR methodology contributes to proactive and efficient detection, facilitating timely interventions and informed management of HPV-related conditions for healthcare professionals.
The CHAINFOR™ HPV ID-26 Screening qPCR Kit stands as an innovative in vitro diagnostic tool, utilizing real-time polymerase chain reaction (qPCR) for the qualitative detection of human papillomavirus (HPV) DNA. This advanced assay is carefully designed to identify 26 high-risk HPV genotypes, including 16, 18, 31, 33, 35, 39, 45, 52, 56, 58, 59, 66, 68, 70, 82, 73, 97, 34, 51, 53, 67, 26, 69, 6, 11, and 30. By offering an extensive range of genotypic coverage, the kit enables precise detection of these HPV types in genomic DNA specimens.
This comprehensive screening tool provides healthcare professionals with valuable information for the early identification of high-risk HPV types associated with potential health risks. The use of sophisticated qPCR technology in the CHAINFOR™ HPV ID-26 Screening qPCR Kit facilitates proactive and accurate detection, thereby contributing to timely interventions and informed management of HPV-related conditions.
The CHAINFOR™ HPV 16/18 Genotyping Detection RT-qPCR Kit is an advanced diagnostic tool designed for the qualitative detection of human papillomavirus (HPV) genotypes 16 and 18. Utilizing real-time reverse transcription polymerase chain reaction (RT-qPCR) technology, this kit allows for the precise identification of these specific high-risk HPV genotypes. With a focus on accuracy and efficiency, the CHAINFOR™ kit offers a comprehensive solution for healthcare professionals, enabling them to detect and differentiate between HPV 16 and 18 in various clinical specimens. This targeted genotyping capability is crucial in assessing the risk of HPV-associated diseases, facilitating early intervention, and guiding informed patient management.
REFERENCES
Ruff, H., Mody, D., Luna, E., Armylagos, D., & Thrall, M. J. (2017). Cervical biopsy rates before and after the introduction of human papillomavirus type reporting in co-tests with negative cytology. Journal of the American Society of Cytopathology, 6(5), 180–184.
Dalton, M. (2023, May 30). HPV (human papillomavirus). NFID. https://www.nfid.org/infectious-disease/hpv/
Mayo Foundation for Medical Education and Research. HPV infection. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/hpv-infection/symptoms-causes/syc-20351596
World Health Organization. Human papillomavirus (HPV). World Health Organization. https://www.who.int/teams/health-product-policy-and-standards/standards-and-specifications/vaccine-standardization/human-papillomavirus
World Health Organization. Human papillomavirus and cancer. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/human-papilloma-virus-and-cancer
Centers for Disease Control and Prevention. (2022, April 12). Std Facts – Human papillomavirus (HPV). Centers for Disease Control and Prevention. https://www.cdc.gov/std/hpv/stdfact-hpv.htm
Centers for Disease Control and Prevention. (2023, February 10). HPV infection. Centers for Disease Control and Prevention. https://www.cdc.gov/hpv/parents/about-hpv.html
HPV and cancer. National Cancer Institute. https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-and-cancer


