ECDC warns of surge in Legionella Disease in Europe. How Common is Legionnaires Disease in Europe?

How Common is Legionella Disease in Europe?
Legionella Disease numbers are sobering. In 2021 alone, Europe witnessed a staggering 10,700 cases. Of these cases, 704 proved fatal. The ECDC’s Annual Epidemiological Report indicated that this surge represented the highest annual notification rate of the disease in the continent, with 2.4 cases per 100,000 population [1].
The surge wasn’t uniform across all regions and demographics. Italy, France, Spain, and Germany accounted for a significant 75 percent of the reported cases [1]. Alarmingly, older males aged 65 years and above bore the brunt of the outbreak, with 8.9 cases per 100,000 population within this demographic [1].

Another recent outbreak of Legionella Disease in south-eastern Poland has resulted in 14 fatalities and more than 150 confirmed cases. The outbreak, detected last week, has led to numerous hospitalizations. Authorities are investigating how the Legionella bacteria, which causes the disease, entered the water supply in the city of Rzeszow and its vicinity. Concerns initially arose due to Rzeszow’s role as a hub for military and humanitarian aid for Ukraine, as well as its hosting of a significant US military presence. However, no evidence of sabotage has been found.
The investigation to determine the outbreak’s cause is ongoing, with initial tests yielding inconclusive results regarding the bacteria’s source. Authorities have responded by adding extra chlorine to the municipal water supply for decontamination and advising residents to boil water before consumption.
The Mystery Behind the Surge : What’s the Cause of the Outbreak?
What makes this surge even more concerning is the lack of a clear-cut explanation. The ECDC cited changes in national testing policies and surveillance systems as potential factors contributing to the increase [2]. An aging population further compounds the problem.
Additionally, changes in the design and infrastructure of water systems, coupled with climate and weather changes, could also be playing a role. These environmental factors may impact both the proliferation of Legionella in the environment and human exposure to water aerosols containing the bacteria.

The surge in Legionnaires Disease cases across Europe is a concerning development that demands urgent attention. While the exact reasons behind this surge are still being investigated, one thing is clear: vigilance is paramount. Public health authorities must remain proactive in their surveillance efforts, and measures to prevent the growth and spread of Legionella bacteria in water systems must be a priority. In an era where we face various health challenges, the rise of Legionnaires Disease reminds us that we must always be prepared to address emerging threats to public health.
ECDC Warns of Surge in Legion Disease in Europe.
In a stark warning, the European Centre for Disease Prevention and Control (ECDC) has raised the alarm about a surging epidemic of Legionnaires Disease sweeping across the European Union (EU) and the European Economic Area (EEA). In its latest Annual Epidemiological Report, the ECDC revealed a staggering total of over 10,700 cases, accompanied by 704 fatalities, in the year 2021 [2] . This concerning surge in cases has catapulted the disease to unprecedented levels, urging health authorities to remain ever vigilant in their efforts to detect and manage outbreaks.

Legionella thrives in specific conditions, such as water temperatures between 25 and 42 degrees Celsius and stagnant water. The ECDC emphasizes the importance of vigilance in detecting clusters and outbreaks through surveillance, given the relatively high mortality rate and the challenges in identifying and controlling environmental sources [2].
What is Legionella Disease?
Legionella Disease (pontiac fever), also known as Legionellosis, is a serious respiratory illness that has captured attention due to its intriguing origins and potentially severe consequences. In this blog, we’ll delve into the fascinating world of Legionella Disease, exploring its history, transmission, symptoms, recent outbreaks and the factors that increase one’s risk of contracting this illness.
Legionella Disease (pontiac fever) earned its name from a notable outbreak at an American Legion convention in Philadelphia in 1976, where many attendees fell ill [1]. The illness was eventually linked to a bacterium called Legionella pneumophila. However, this bacterium and the disease it causes have been around much longer. Here’s a brief historical overview:
Legionella bacteria were first discovered in 1977 when they were isolated from the lungs of deceased Legionnaires [1]. Legionella naturally exists in water sources, like rivers and lakes, but it’s when these bacteria find their way into human-made water systems that problems can arise.
How is Legionella Disease Spread?
Legionella Disease (pontiac fever) is not spread from person to person. Legionnaires Disease primarily spreads through the inhalation of aerosolized water droplets contaminated with Legionella bacteria [1]. The sources of these contaminated droplets are varied:
Water Systems: Legionella can proliferate in human-made water systems such as cooling towers, hot water tanks, plumbing systems, and decorative fountains. Inhalation of water vapor from these systems poses a risk.

Showers and Faucets: Even taking a shower or using a faucet can pose a risk if the water system is contaminated. Although the risk is lower compared to large cooling towers, it’s still possible.
Aspiration: In rare cases, Legionella can be aspirated (inhaled into the lungs) when contaminated water enters the airway while drinking or swallowing.
What are the Symptoms of Legionella Diseases?
Legionella Diseases shares symptoms with other forms of pneumonia, which can make it challenging to diagnose. Common symptoms include:
High Fever: Often the first noticeable symptom, with temperatures exceeding 39°C (102°F).
Cough: Initially, it may be dry but can progress to a productive cough with mucus.
Shortness of Breath: Breathlessness, especially during physical activity.

Muscle Aches and Fatigue: Generalized body aches and feeling extremely tired.
Headache: Sometimes severe.
Gastrointestinal Symptoms: Nausea, vomiting, and diarrhea can occur but are less common.
The incubation period, or the time from exposure to symptoms, is usually 2 to 10 days [1].
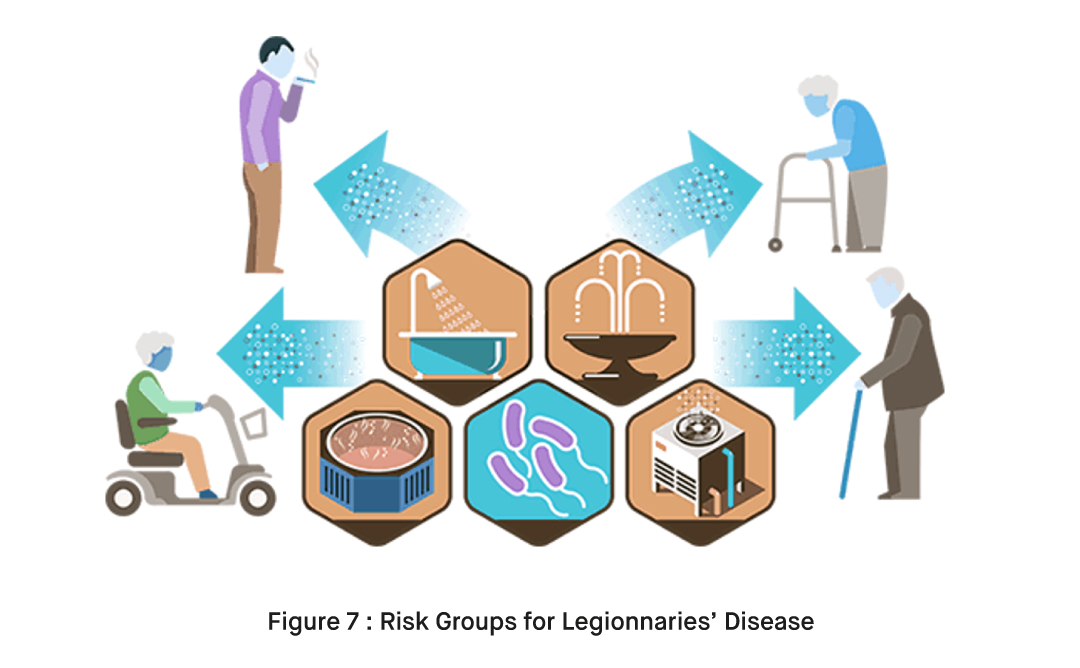
What are the Risk Factors for Legionnaires Disease?
Certain factors can increase the risk of contracting Legionnaires Disease. These include age (older adults are more susceptible), smoking, weakened immune systems, chronic lung diseases, and certain medical conditions or treatments that weaken the immune system [3].
Not everyone exposed to Legionella bacteria will become ill; however, Legionnaires Disease can be severe and even fatal, especially in individuals with underlying health conditions.
Age: Older adults, particularly those over 50, are at higher risk, as are individuals with weakened immune systems.
Smoking: Current or past smoking increases vulnerability to respiratory infections, including Legionnaires Disease.
Underlying Health Conditions: Conditions like chronic lung disease, diabetes, kidney disease, and cancer can weaken the immune system.
Immunosuppressive Medications: Medications that suppress the immune system, often prescribed after organ transplants or for autoimmune diseases, can increase susceptibility.
Travel and Exposure: Staying in hotels or facilities with contaminated water systems, especially in high-risk areas, can increase exposure.
Legionnaires Disease is a formidable illness with a storied history and a complex mode of transmission. Understanding its origins, transmission routes, symptoms, and risk factors is crucial for prevention and early detection. If you or someone you know exhibits symptoms consistent with Legionnaires Disease, seeking prompt medical attention is essential, particularly if you have known risk factors. Public health measures, such as proper water system maintenance and surveillance, also play a pivotal role in reducing the risk of Legionella outbreaks and protecting public health.
What are the Diagnostic Methods for Legionella Diseases?
Diagnosing Legionella Diseases typically involves a combination of clinical evaluation, laboratory tests, and sometimes imaging studies. Legionnaires Disease is caused by the bacterium Legionella pneumophila, and early diagnosis is crucial for effective treatment. Here are the main diagnostic methods for Legionnaires Disease:
- Clinical Evaluation:
– Symptoms: Legionnaires Disease often presents with symptoms similar to pneumonia. Common symptoms include high fever, cough, shortness of breath, muscle aches, headache, and chest pain. Gastrointestinal symptoms, such as diarrhea and nausea, may also occur.
– Physical Examination: Healthcare providers may perform a physical examination to assess vital signs, listen to lung sounds, and check for signs of pneumonia.
- Laboratory Tests:
– Urine Antigen Test: This is one of the most common and rapid diagnostic tests for Legionnaires Disease. It detects a specific antigen (a substance produced by the bacterium) in a urine sample.
– Sputum Culture: A sputum sample may be collected and sent for bacterial culture. This can help identify the presence of Legionella bacteria in the respiratory tract, but it takes longer to obtain results compared to the urine antigen test.
– Blood Tests: Blood tests, such as a complete blood count (CBC) and serum electrolytes, can help assess the severity of the infection and its impact on the body.

- Chest X-ray or CT Scan:
– Imaging studies, such as a chest X-ray or a computed tomography (CT) scan, may be performed to visualize the lungs and assess the extent of lung involvement. This can help differentiate Legionnaires Disease from other respiratory conditions.
- Bronchoscopy:
– In some cases, a bronchoscopy may be performed to collect samples from the lower respiratory tract. This procedure involves inserting a thin, flexible tube with a camera into the airways to obtain samples for culture and testing.
- Serologic Testing:
– Serologic tests measure the presence of antibodies against Legionella in the patient’s blood. These tests may be used in some cases, but they are less commonly employed than the urine antigen test because they are less specific and can take several weeks to show results.
- Polymerase Chain Reaction (PCR) Testing:
– PCR testing can detect Legionella DNA in respiratory secretions or tissue samples. It is a sensitive method for confirming the presence of the bacterium.
Diagnosis of Legionnaires Disease often involves a combination of these methods. The urine antigen test is particularly valuable due to its rapid results and high sensitivity. Prompt diagnosis and treatment with antibiotics, such as azithromycin or levofloxacin, are essential to improve outcomes for patients with Legionnaires Disease. If you suspect you have Legionnaires Disease or have been exposed to contaminated water sources, it is important to seek medical attention promptly.
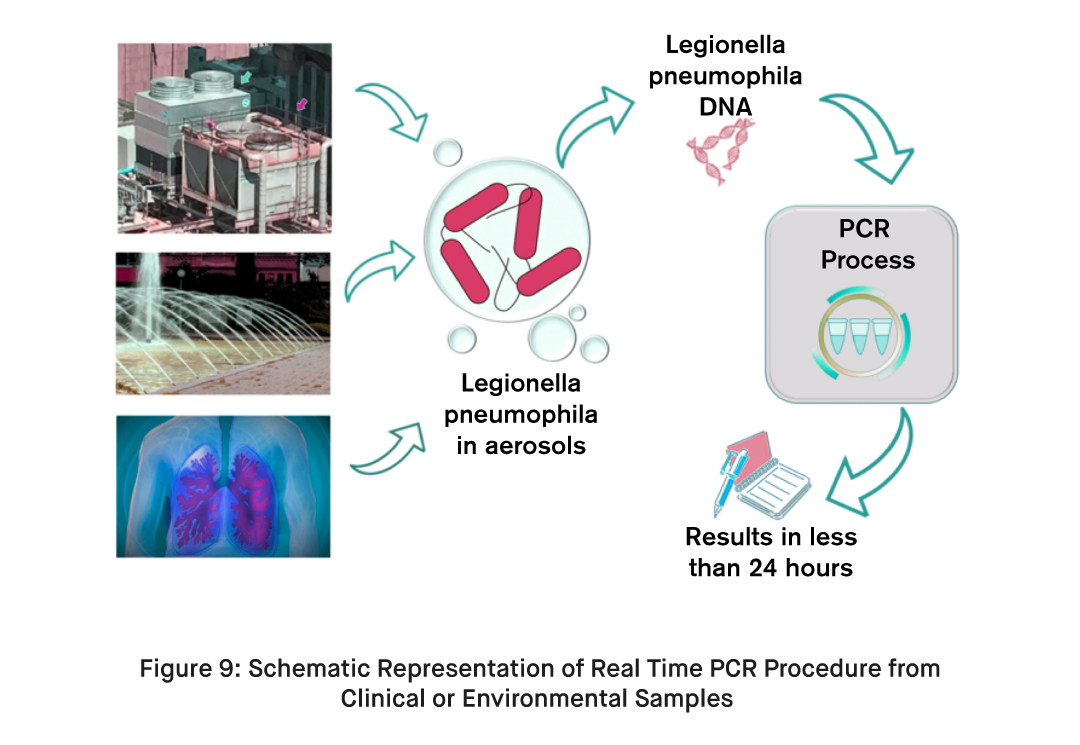
How to Use Legionella Pneumophila Real Time PCR Detection Kit?
Using a Legionella pneumophila Real-Time PCR Detection Kit involves molecular techniques to detect the DNA of Legionella pneumophila, the bacterium responsible for causing Legionnaires Disease, in clinical or environmental samples. These kits are typically used in laboratories with expertise in molecular biology and PCR techniques. Here are the general steps for using a Legionella pneumophila Real-Time PCR Detection Kit:
It’s crucial to follow the manufacturer’s instructions provided with the specific PCR kit you are using, as there may be variations in the protocol. Additionally, proper laboratory safety procedures and aseptic techniques should always be followed.
Materials Needed
- Legionella pneumophila Real-Time PCR Detection Kit
- Sample containing Legionella DNA (e.g., clinical sample, water sample)
- PCR thermal cycler
- Pipettes and tips
- Nucleic acid extraction kit (if necessary for sample preparation)
- Reaction tubes or plates
- Positive and negative controls
- Laboratory safety equipment (e.g., lab coat, gloves, safety goggles)
Procedure:
- Sample Preparation:
– If you are working with a clinical sample, extract DNA from the sample using a suitable nucleic acid extraction kit following the manufacturer’s instructions.
– For environmental water samples, concentrate or filter the sample to collect Legionella bacteria and their DNA.
- Setting up the Reaction:
– Prepare a PCR reaction mix according to the kit’s instructions. The reaction mix typically contains PCR buffer, primers, probes, DNA polymerase, and other necessary components.
– Include positive and negative controls in your experiment to ensure the accuracy of the results.
- Sample Addition:
– Add a specific volume of your extracted DNA (or concentrated sample) to the reaction mix. The kit’s instructions will specify the volume of DNA to add.
- PCR Thermal Cycling:
– Place the reaction tubes or plates in a PCR thermal cycler.
– Set the cycling conditions according to the kit’s instructions, including the annealing temperature, extension time, and number of cycles.
– Real-time PCR instruments will continuously monitor the amplification of DNA during the cycling process.
- Data Analysis:
– After the PCR is complete, analyze the real-time PCR data using the software provided with your PCR instrument.
– Interpret the results based on the fluorescence signal. The presence or absence of a fluorescent signal in the amplification curve will indicate the presence or absence of Legionella pneumophila DNA in the sample.
- Result Interpretation:
– Compare the sample’s amplification curve to those of the positive and negative controls.
– A positive result will show a characteristic amplification curve, while a negative result will show no or minimal amplification.
– Quantification may also be possible, depending on the kit used.
- Reporting and Documentation:
– Document the results, including the cycle threshold (Ct) values if quantification is performed.
– Interpret the results in the context of clinical or environmental significance.
Always follow the specific instructions provided by the kit manufacturer and adhere to standard laboratory safety practices when performing PCR experiments. If you are not trained in molecular biology techniques, consult a laboratory professional or molecular biologist for guidance.
How to Use Legionella Diseases Rapid Test Kit?
Legionella Disease rapid test kits are designed to detect specific antigens produced by the Legionella bacteria in urine samples. These kits are commonly used in clinical settings to quickly diagnose the disease. It’s essential to follow the manufacturer’s instructions provided with the specific test kit you are using, as instructions may vary slightly between different kits. However, here are general steps for using a Legionnaires Disease rapid test kit:
- Gather Supplies:
– Legionnaires Disease rapid test kit
– Clean and dry urine collection container
– Personal protective equipment (PPE), such as disposable gloves
- Prepare the Patient:
– Ensure the patient has not urinated for at least 2-4 hours before the test to obtain a concentrated urine sample.
– Explain the procedure to the patient and obtain their informed consent if required.
- Wear PPE:
– Put on disposable gloves to prevent contamination.
- Collect Urine Sample:
– A urine sample is collected from the patient. This is typically a midstream urine sample obtained under sterile conditions.
– The volume of urine required may vary depending on the specific test kit, so follow the kit’s instructions regarding the amount of urine needed.

- Perform the Test:
– Open the Legionnaires Disease rapid test kit, ensuring you follow any specific storage or handling instructions provided by the manufacturer.
– Carefully read and follow the kit’s instructions for inserting the urine sample into the test device.
– Typically, you will add a few drops of the urine sample to a designated area on the test device or dip a test strip into the urine sample.
– Be cautious not to touch the test area with your fingers or any contaminated surfaces to avoid false results.
- Wait for Results:
– Allow the test to run for the specified amount of time, as indicated in the kit’s instructions. This time may vary but is usually around 15-30 minutes.
– During this waiting period, do not disturb the test device or manipulate the sample.
- Interpret the Results:
– After the specified time, observe the test device for the appearance of lines, colors, or other indicators. Most test kits will provide clear instructions on how to interpret the results.
– The presence or absence of specific lines or colors on the test device will indicate whether Legionella antigens were detected in the urine sample.
- Document the Results:
– Record the test results, including whether the test is positive or negative, the date, and any other relevant information.
– If the test is positive, consult a healthcare provider for further evaluation and treatment.
- Dispose of Materials:
– Dispose of used gloves, urine collection container, and any other disposable materials according to proper medical waste disposal guidelines.
Always follow the manufacturer’s instructions and adhere to standard laboratory and safety protocols when using a Legionnaires Disease rapid test kit. If you are not trained in medical testing procedures, consult a healthcare professional or laboratory technician for guidance.
REFERENCES
[1] Legionellosis (Legionnaires’ Disease and Pontiac Fever) – Overview | Occupational Safety and Health Administration. (n.d.). Legionellosis (Legionnaires’ Disease and Pontiac Fever) – Overview | Occupational Safety and Health Administration. https://www.osha.gov/legionnaires-disease
[2] Facts about Legionnaires’ disease. (2012, May 31). European Centre for Disease Prevention and Control. https://www.ecdc.europa.eu/en/legionnaires-disease/facts
[3] Legionnaires Disease Specifics For Clinicians | CDC. (2021, March 25). Legionnaires Disease Specifics for Clinicians | CDC. https://www.cdc.gov/legionella/clinicians/disease-specifics.html


