Spring brings renewal but also triggers allergic disease in millions globally. Allergic rhinitis, allergic asthma, and atopic dermatitis peak during pollen season, affecting primary care systems and patient quality of life. A blood test measuring quantitative total immunoglobulin E (total IgE) provides biomarker information about atopic disease and may assist in determining eligibility for targeted anti-IgE therapy such as omalizumab. Point-of-care quantitative IgE testing, completed in 15 minutes, enables primary care clinicians to obtain biomarker measurements without laboratory delays.
Allergic Disease: A Growing Global Burden Peaking Every Spring
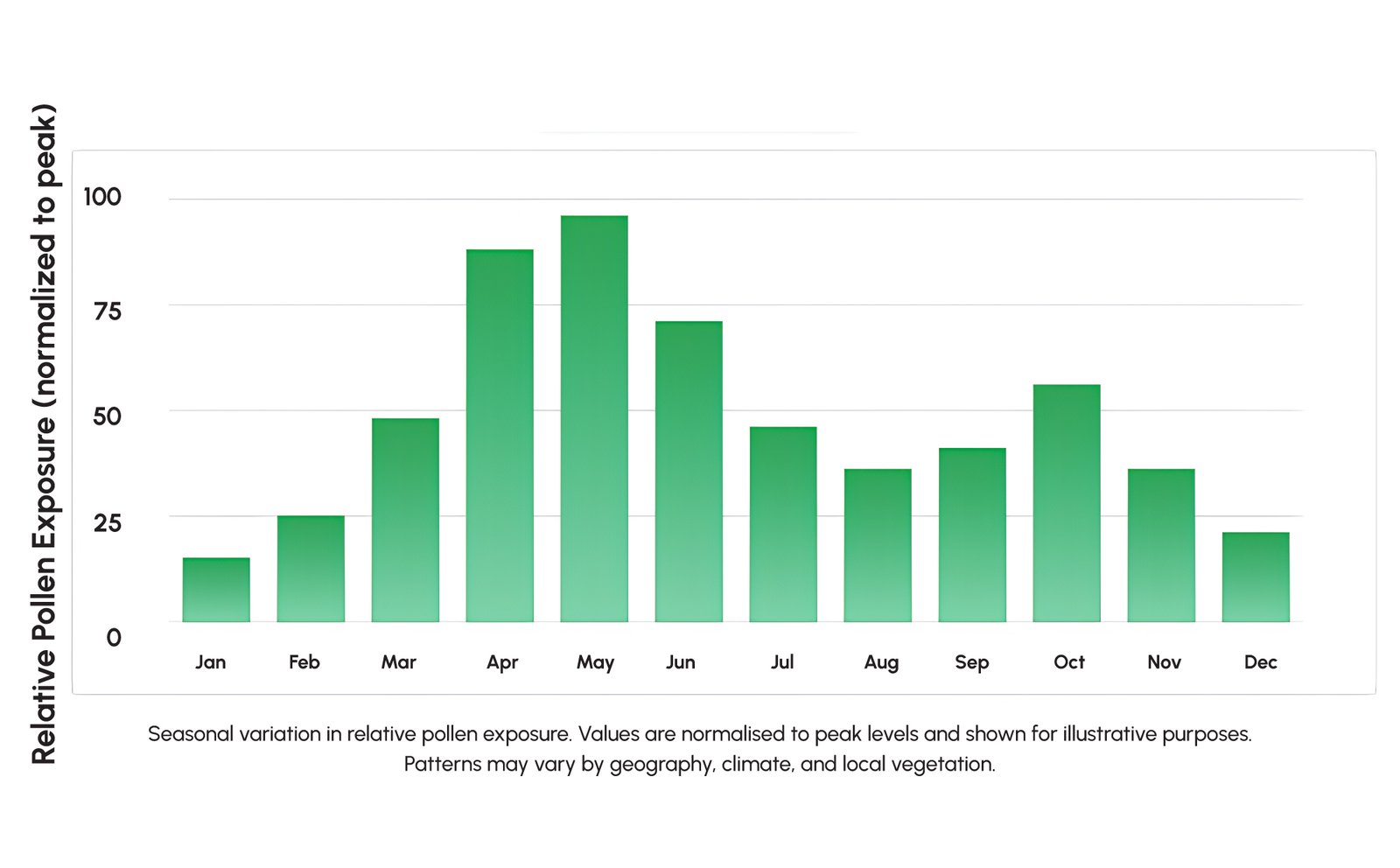
Allergic diseases represent a substantial public health consideration worldwide. Allergic diseases affect a significant portion of the global population, making allergy one of the most common chronic conditions in developed nations. Allergic rhinitis (hay fever) affects hundreds of millions of people globally, making it one of the most common allergic diseases. In the Northern Hemisphere, spring represents a peak period of allergic disease presentation, driven by the release of tree pollens (birch, oak, ash) in early spring (March to April) and grass pollens in late spring and early summer (May to June). The timing of the pollen season varies geographically but, across temperate zones, creates a predictable pattern of allergic rhinitis symptoms, allergic asthma presentations, and atopic dermatitis flares during these months.
The prevalence of allergic disease has increased in recent decades, a trend attributed to various factors including the hygiene hypothesis (reduced early-life microbial exposure), rapid urbanisation, air pollution, and climate change. Rising global temperatures may extend pollen seasons, increase pollen production per plant, and alter plant phenology, creating longer periods of allergen exposure. Air pollution may exacerbate allergic airway inflammation. The economic burden of allergic disease is substantial. In the United States, allergic rhinitis costs the healthcare system over 24 billion dollars annually in direct medical costs and indirect costs from lost productivity (American Academy of Allergy, Asthma and Immunology, 2023). Individuals with allergic rhinitis may experience reduced cognitive function, impaired sleep quality, and decreased work and academic performance.
Beyond allergic rhinitis, spring allergy season is associated with presentations of allergic asthma. The relationship between allergic rhinitis and asthma is well established, with many patients with asthma also experiencing allergic rhinitis. Atopic dermatitis (eczema), another IgE-mediated condition, may show seasonal fluctuation in symptom severity. Additionally, food allergy and drug allergy, though less directly seasonal, may coexist with seasonal allergic diseases in patients with underlying atopic phenotype. The atopic march describes the tendency for individuals with one allergic disease to develop others sequentially. For example, infants with atopic dermatitis may have higher risk of developing allergic rhinitis and asthma later in childhood. Identifying atopic individuals through biomarker testing may provide information for clinical assessment.
The Immunology of Allergy: Why Total IgE Is a Biomarker
Immunoglobulin E (IgE) is the least abundant immunoglobulin in human serum, comprising less than 0.001 per cent of total serum protein under normal conditions, with typical adult serum concentrations of 0 to 100 IU/mL (international units per millilitre). Despite its minute concentration, IgE plays a role in both the protective immune response against parasitic infections and the response in allergic disease. In non-sensitised individuals, serum IgE levels remain low and stable. However, in individuals with genetic and environmental predisposition to atopy, exposure to allergen triggers T-helper 2 (Th2)-driven immune responses characterised by interleukin-4 (IL-4) and IL-5 production, which stimulate B cells to produce allergen-specific IgE. This allergen-specific IgE binds to high-affinity IgE receptors (FcεRI) on the surface of tissue-resident mast cells and circulating basophils.
Upon re-exposure to allergen, cross-linking of FcεRI-bound IgE by the allergen triggers mast cell and basophil degranulation with release of pre-formed mediators (histamine, tryptase, heparin) and newly synthesised mediators (leukotrienes, prostaglandins, cytokines, chemokines). This immunological cascade is the basis of the immediate hypersensitivity reaction. In allergic rhinitis, allergen-induced degranulation of nasal mast cells is associated with nasal edema, mucus production, and pruritus. In allergic asthma, mast cell and eosinophil mediators are associated with airway smooth muscle constriction and inflammation. Total serum IgE reflects the overall burden of allergen-specific IgE across all allergen specificities. An elevated total IgE level suggests underlying atopic sensitisation but does not identify which specific allergen or allergens are involved. For allergen-specific identification, allergen-specific IgE testing (ImmunoCAP) or skin prick testing is required. However, total IgE serves as a screening biomarker for atopic disease and provides information for clinical assessment.
Causes of elevated total IgE extend beyond allergic disease. Parasitic infections, particularly helminth infections common in tropical regions, drive strong Th2 responses and may elevate total IgE levels. Certain primary and secondary immunodeficiency states, such as ataxia telangiectasia and selective IgA deficiency, are associated with elevated IgE. Non-allergic causes of inflammation, such as some malignancies and post-transplant lymphoproliferative disorder, can elevate IgE. Hyper-IgE syndromes are rare genetic conditions characterised by markedly elevated total IgE levels (often greater than 2,000 IU/mL) and susceptibility to recurrent infections. In clinical practice, total IgE greater than 150 IU/mL in adults and age-adjusted thresholds in children is generally considered elevated and warrants further clinical evaluation. Normal total IgE does not exclude allergic disease, particularly local allergic rhinitis, which is characterised by local nasal IgE production despite normal serum total IgE. Nevertheless, total IgE provides information in the assessment of suspected allergic disease.

Point-of-Care Total IgE in Clinical Practice: From Allergy Screening to Therapy Monitoring
Total IgE point-of-care testing provides biomarker measurement across multiple clinical settings. In primary care, a clinician encountering a patient with suspected allergic rhinitis, allergic asthma, or atopic dermatitis can perform POC total IgE testing to obtain biomarker information about atopic status. An elevated total IgE on POC testing provides information that may support the clinical assessment of allergic disease and inform referral decisions to allergy specialists. In paediatric practice, POC total IgE testing provides biomarker information in assessing children with atopic presentations. An infant presenting with atopic dermatitis can be tested for elevated IgE, and if elevated, this information may inform clinical surveillance and management decisions. In pulmonary medicine, total IgE testing helps characterise asthma by identifying the allergic component of disease, which is relevant for therapy selection. Patients with allergic asthma may be candidates for targeted anti-IgE therapy (omalizumab) if they meet criteria, making total IgE measurement part of the pre-treatment evaluation.
In emergency medicine, POC total IgE can provide biomarker information in the investigation of allergic presentations. Although acute serum IgE measurement is not routinely used to diagnose acute anaphylaxis (clinical diagnosis is made on presentation), measuring total IgE in the patient with suspected atopic disease who presents with anaphylaxis provides background information for long-term management planning. In travel medicine and tropical medicine, elevated total IgE in a returning traveller may prompt investigation for parasitic infection, particularly helminth infections. Serological parasitic testing can then be targeted based on exposure history and epidemiology. The practical workflow in primary care is straightforward: collect whole blood or serum for POC total IgE testing, obtain a result in 15 minutes, and use the result to inform clinical assessment and referral decisions. An elevated total IgE (greater than 100 IU/mL in adults, age-adjusted in children) may inform referral for allergen-specific IgE panel or skin prick testing. If clinical suspicion for parasitic infection exists (traveller from endemic area with unexplained eosinophilia and elevated IgE), specific parasitic serology can be ordered.
The most important clinical use of total IgE in primary and secondary care is pre-treatment evaluation for omalizumab (anti-IgE monoclonal antibody). Omalizumab is indicated for moderate to severe allergic asthma and for severe atopic dermatitis. Omalizumab dosing is calculated based on the baseline total IgE level and body weight, using published dosing tables. Patients with total IgE levels outside the dosable range are not eligible for treatment. A baseline total IgE measurement is therefore required before omalizumab initiation. Some clinicians measure total IgE during omalizumab therapy to monitor biomarker levels. In clinical research and specialised immunodeficiency clinics, total IgE monitoring is used for assessment purposes.
The Vitrosens RapidFor™ Total IgE FIA Platform
The RapidFor™ Total IgE (FIA) is a quantitative fluorescence immunoassay for the measurement of total immunoglobulin E in human whole blood, serum, or plasma, operated on the FIAPro™ Analyzer System. The assay covers a clinical measurement range of 20 to 4,000 IU/mL with a turnaround time of 15 minutes. With age-specific reference ranges for paediatric populations and regulatory approval for clinical IVD use, it provides biomarker measurement for allergic and atopic disease assessment across primary care and specialist settings.
Ref. No |
Name |
Specimen Type |
Turnaround Time |
Reference Range |
Linearity Range |
Regulatory Status |
VMPO79 |
Total IgE |
Serum/Plasma/Whole Blood |
15 minutes |
Adults: 0-100 IU/mL (age-specific ranges for children) |
20 – 4,000 IU/mL |
CE, MHRA |
Key Features and Benefits:
The assay provides a quantitative total IgE measurement range of 20 to 4,000 IU/mL, covering a broad spectrum of atopic conditions from mild elevation to severe disease. A 15-minute turnaround time from whole blood enables same-visit clinical decision-making, while age-specific reference ranges support appropriate interpretation across neonatal, paediatric, and adult populations. Compatibility with whole blood, serum, and plasma allows use in a wide range of clinical settings, and the test supports baseline IgE assessment prior to initiating therapies such as omalizumab in patients with moderate to severe allergic disease.

From Screening to Specialist Referral: Building an Allergy Pathway with POC IgE
Spring allergy season places pressure on primary care systems as patients present with allergic rhinitis, allergic asthma presentations, and allergic conjunctivitis. Many primary care clinicians manage allergy symptomatically with antihistamines and intranasal corticosteroids without performing biomarker assessment. However, evidence supports identification of atopic disease through biomarker measurement, as this provides information for clinical assessment and referral decisions. POC total IgE testing provides a mechanism for biomarker measurement in the primary care setting. A patient presenting with seasonal allergic rhinitis symptoms can undergo POC total IgE testing during the visit. If elevated, this information may inform referral to allergy specialist for allergen-specific IgE testing.
In paediatric practice, POC total IgE testing enables identification of the atopic phenotype in children with atopic dermatitis or allergic symptoms. Recognition of atopy through biomarker testing provides information for clinical management including allergen avoidance strategies, optimised skin care, and surveillance for food allergy development. Children with significantly elevated total IgE (greater than 150 IU/mL) and severe atopic dermatitis may warrant more intensive investigation for food allergy. The global burden of atopic disease and the predictable spring seasonal pattern creates opportunities for allergy screening and pathway development. Health systems implementing POC allergy biomarker testing during spring months can identify patients with elevated biomarkers and streamline specialist referrals.
For patients with established allergic asthma, POC total IgE measurement provides information for therapy eligibility assessment. Omalizumab (Xolair), an anti-IgE biologic therapy approved for allergic asthma, works by binding circulating free IgE. Omalizumab is indicated for patients with moderate to severe allergic asthma. Total IgE measurement is required for patient selection and dosing. A baseline POC total IgE result enables primary care clinicians to obtain this biomarker information and facilitate specialist referral when appropriate. More recently, dupilumab (IL-4 receptor antagonist) has been approved for allergic asthma, allergic rhinitis, and atopic dermatitis, and other biologics targeting Th2 pathways are in development or approval. While these newer agents do not require total IgE dosing, total IgE provides biomarker information about underlying atopic inflammation.
Clinical Applications of POC Total IgE Testing:
- POC total IgE testing in primary care during spring allergy season provides biomarker measurement and may inform specialist referral decisions
- Age-specific reference ranges support detection of atopic phenotype in children, providing information for clinical assessment and surveillance
- Baseline total IgE measurement is required for omalizumab eligibility assessment in patients with moderate-severe allergic asthma
- Serial total IgE measurement during anti-IgE therapy provides biomarker information that may inform therapy monitoring in specialist settings
- POC total IgE testing in travel medicine and tropical medicine provides biomarker information for identifying parasitic infection risk in returning travellers
Conclusion
Allergic diseases represent a substantial global health consideration, with predictable seasonal patterns during spring pollen season. Total IgE is a biomarker of underlying atopic sensitisation and provides information for clinical assessment, specialist referral decisions, and therapy selection. Quantitative point-of-care total IgE testing, completed in 15 minutes from whole blood, enables primary care clinicians to obtain biomarker measurements without delays for laboratory processing. For patients with established allergic asthma, baseline total IgE measurement is required for determining omalizumab eligibility and calculating appropriate dosing.
The RapidFor™ Total IgE (FIA) platform brings quantitative IgE measurement to the point of care, with CE and MHRA approval for clinical use. Its 20 to 4,000 IU/mL measurement range, age-specific reference ranges, rapid 15-minute turnaround, and specimen flexibility make it suitable for primary care allergy screening, paediatric atopy assessment, emergency evaluation of allergic presentations, and pre-treatment biomarker evaluation for omalizumab and other IgE-targeted therapies. By providing access to quantitative IgE measurement, POC platforms offer biomarker information that may support clinical assessment and evidence-based allergy management across primary, secondary, and tertiary care.
Visit vitrosens.com or contact sales@vitrosens.com to learn more about the RapidFor™ Total IgE FIA platform and how point-of-care IgE testing can be integrated into your allergy assessment and management pathway.
References
- Pawankar R, Canonica GW, Holgate ST, Lockey RF (Eds.). (2013). World Allergy Organization (WAO) White Book on Allergy: Executive Summary. World Allergy Organization Publications.
- Platts-Mills TAE. (2015). The allergy epidemics: 1870-2010. Journal of Allergy and Clinical Immunology, 136(1), 3-15.
- Galli SJ, Tsai M, Piliponsky AM. (2008). The development of allergic inflammation. Nature, 454(7203), 445-454.
- Amin HS, Liss GM, Bernstein DI. (2004). Evaluation of near-patient testing for total serum IgE. Allergy, 59(6), 584-589.
- Humbert M, Beasley R, Ayres J, et al. (2005). Benefits of omalizumab as add-on therapy in patients with severe persistent allergic asthma. American Journal of Respiratory and Critical Care Medicine, 172(10), 1378-1389.
- American Academy of Allergy, Asthma and Immunology. (2023). Allergy Statistics. AAAAI Publications.
- Matricardi PM, Kleine-Tebbe J, Hoffmann HJ, et al. (2016). EAACI Molecular Allergology User’s Guide. Pediatric Allergy and Immunology, 27(Suppl 23), 1-250.
- Bousquet J, Khaltaev N, Cruz AA, et al. (2008). ARIA: Allergic Rhinitis and its Impact on Asthma. Journal of Allergy and Clinical Immunology, 122(Suppl 2), S1-S84.
- Sears MR. (2015). Epidemiology of childhood asthma. Lancet, 368(9537), 763-770.
- Schleich FN, Sele J, Seidel L, et al. (2017). Clusters of comorbidities in adult asthma phenotypes. Data from the COBRA study. Respiratory Medicine, 117, 1-7.
- Renz H, Skoner D. (2003). Relations between infection and allergic inflammation: Epidemiology, mechanisms, and therapeutic implications. Journal of Allergy and Clinical Immunology, 111(3), 534-540.
- Holgate ST. (2008). Pathogenesis of allergic and non-allergic rhinitis. Clinical and Experimental Allergy, 38(10), 1554-1567.


