Monkeypox Virus: Is the new pandemic coming?

The recent outbreaks of the monkeypox virus in several non-endemic countries have sparked widespread worry throughout the world and stirred questions about whether we are about the face with a new pandemic. According to the latest data by World Health Organization (WHO), as of May 22, more than 250 confirmed and suspected cases have been officially reported from 16 countries and several WHO regions. Read along to learn more about the risk assessment of monkeypox disease and expert opinion on whether it may cause a new pandemic. You can also access the latest updates on monkeypox by visiting the websites of institutions such as WHO, CDC, and ECDC.
What is Monkeypox?
Known as a less lethal and infectious relative of the smallpox virus, monkeypox virus is an enveloped double-stranded DNA virus from the Ortho-poxvirus genus in the family Poxviridae. Caused by infection with monkeypox virus, monkeypox is a zoo-tonic disease with signs and symptoms similar to that of smallpox. Monkeypox transmits mainly through contact with blood, bodily fluids, and lesion material of infected animals and humans, or with contaminated materials.
Although its main hosts are thought to be rodents, the monkeypox virus was named after its initial discovery in 1958 in colonies of monkeys used for research. In 1970, the first human case of monkeypox was detected in the Democratic Republic of Congo during a period in which the efforts for eradicating smallpox were at its peak. Following its discovery, the spread of monkeypox virus had been limited to tropical rainforest regions of Central and West Africa until 2003. Even after 2003, while the virus was occasionally transported to other areas via international trade or travel, its spread was quickly contained.
What are the symptoms of monkeypox?

The symptoms of monkeypox are similar to those of smallpox. Fever, headache, muscle aches, back pain, swollen lymph nodes, chills, and exhaustion are the first symptoms. A rash usually appears 1 to 5 days after the initial symptoms and spreads throughout the body. The rash gradually progressed from small blisters to scabs before falling off. The incubation period is 5 to 21 days between initial contact and the onset of symptoms, and symptoms typically last 2 to 4 weeks.
Are monkeypox breakouts common?
Since the identification of the first human case in the Republic of the Congo in 1970, the virus has mostly affected populations in rural and tropical regions in Central and Western Africa, with human cases reported in 11 African countries including the Democratic Republic of the Congo, Nigeria, Cameroon, the Central African Republic, Benin, Liberia, Gabon, Sierra Leone, Côte d’Ivoire, South Sudan, and the Republic of the Congo. While monkeypox has been rarely spotted outside of these 11 African countries, breakouts elsewhere have occasionally occurred. The first monkeypox outbreak in the Western Hemisphere occurred in the US in 2003, when pet prairie dogs imported from Ghana. With a case count of more than 70 human cases, this was the largest outbreak until 2022. More recently, monkeypox cases linked to international travel have been reported in Israel (2018), Singapore (2019), the UK (2018 and 2019), and the US (2021). Altogether, although rare, breakouts within non-endemic countries have occurred in the past, and each breakout have been quickly contained.
What’s different about the current monkeypox outbreaks?

The current monkeypox outbreak is unusual is that for the first time an outbreak involves many infections happening concurrently outside of the African countries where the disease is endemic. Indeed, as of May 23, the disease has spread across 16 non-endemic countries including the UK, Spain, Portugal, Canada, Italy, Belgium, Germany, Australia, Netherlands, the US, Austria, Denmark, France, Israel, Sweden, and Switzerland.
What about previous monkeypox cases?
In the past, monkeypox cases in non-endemic countries also involved little to no human-to-human transmission and could be linked to infected animals or international travel. Unlike prior instances, many of the people infected during the current monkeypox breakout do not have a history of recent travel to Africa or known exposure to an infected person or animal.
How does monkeypox spread?

Close contact with infected animals and humans, as well as contaminated materials, spreads the monkeypox virus. The virus can enter the body through open wounds, the respiratory tract, and mucous membranes such as the eyes, nose, and mouth.
Animal-to-human transmission of monkeypox may occur through contact with an infected animal’s blood, bodily fluids, and lesion material, including wounds such as bites and scratches. Consuming undercooked meat and other products from infected animals is also thought to be a possible source of contamination.
Is it true that monkeypox can be spread by respiratory droplets?
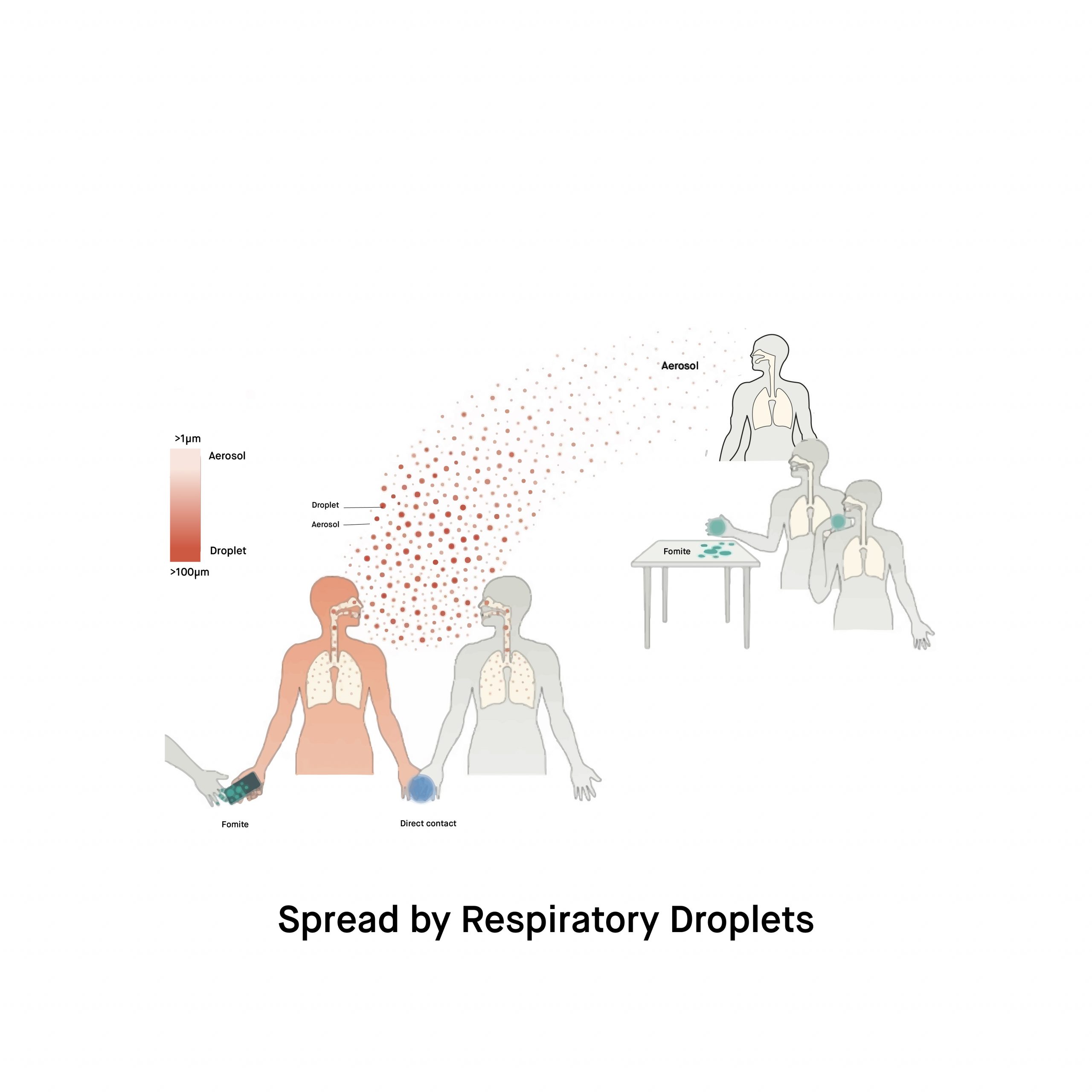
The answer is simply yes. Contact with an infected person’s respiratory secretions, bodily fluids, and skin lesions can result in human-to-human transmission. Contact with recently contaminated objects can also result in transmission. Aside from close contact, monkeypox can be transmitted from mother to fetus via the placenta. While close physical contact has been identified as a transmission route, data is insufficient to determine whether monkeypox spreads directly through sexual intercourse.
How fast does monkeypox spread from human to human?
Monkeypox is a human communicable disease. Only limited human-to-human transmission has previously been reported, with estimated transmission rates ranging from 3.3 percent to 30 percent; however, during a recent outbreak in the Democratic Republic of the Congo, the transmission rate was estimated to be 73%. Infected people may be contagious for up to 21 days after the rash appears, or until all skin lesions have formed scabs and no other symptoms are present.
Monkeypox goes global: why scientists are on alert?
Some people, such as children, pregnant women, and the immunocompromised, can develop more severe illness. The true scope of monkeypox is unknown. Nonetheless, the virus has been linked to deaths in Africa, with a fatality rate of up to one in ten infected people. Future research is needed to determine the exact risks and risk groups associated with monkeypox disease.
Is monkeypox going to be the next pandemic?

In general, experts agree that there is no reason to think that monkeypox could cause a pandemic for the moment, and claim that unless significant upsurge of cases, events, and ongoing transmission are observed, broad preventive measures are not likely to be necessary.
First, the monkeypox virus is significantly less transmissible than viruses such as smallpox and measles, and much less transmissible than SARS-CoV-2. Research investigating whether the virus causing the current outbreak might have undergone mutations that could make it more infectious is ongoing, however the early results illustrate no evidence of such mutation. In May 23, CDC officials reported that viral sequences isolated from the current outbreak looked very similar to those from West African cases, with no evidence of a mutation improving human-to-human transmission. Thus, for the moment, it is safe to say that the virus does not spread easily among people, and the overall risk of transmission for the public remains low. The monkeypox virus is also not considered infectious before the onset of symptoms, which would break the of transmission by allowing timely recognition and containment.
Finally, and perhaps most importantly, the monkeypox virus is unlikely to cause a pandemic because we are already known much about the virus, its behavior, and its primary modes of transmission. Treatments and highly efficient vaccines have already been developed and are ready to be used to protect those at high risk from infection and severe disease. Altogether, public health authorities are already much better equipped to fight against a potential threat of monkeypox than they have been for COVID-19 at the onset of the pandemic.


