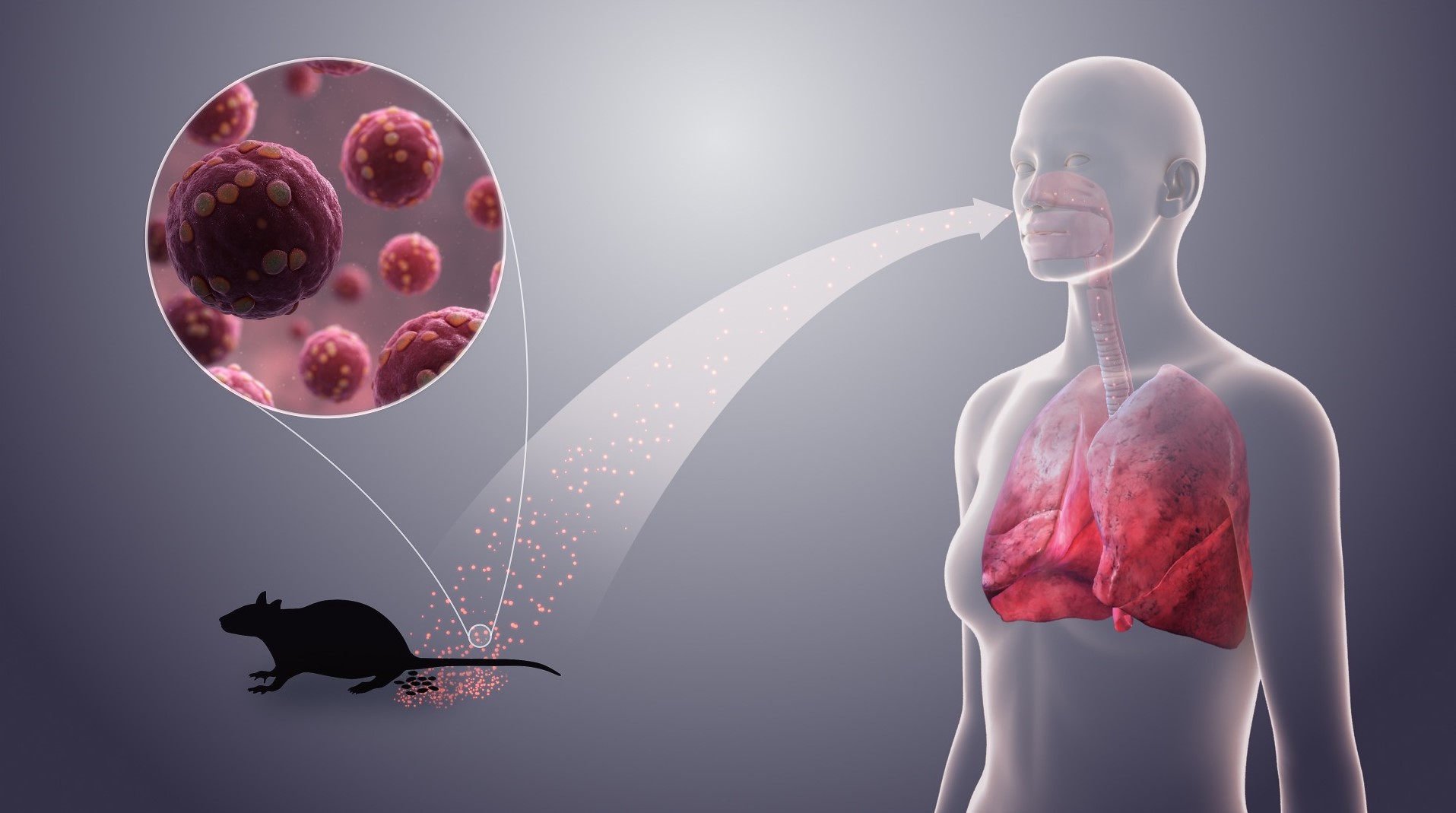
Hantaviruses are a group of zoonotic viruses carried mainly by rodents. Although relatively rare, they can lead to serious and sometimes fatal diseases. According to recent World Health Organization (WHO) outbreak reports published yesterday, hantaviruses may cause different clinical syndromes depending on the virus type and geographic region. In America, hantavirus infection is mainly associated with hantavirus cardiopulmonary syndrome (HCPS/HPS), while in Europe and Asia it is more commonly linked to hemorrhagic fever with renal syndrome (HFRS).
Recent Outbreak Investigation on the MV Hondius
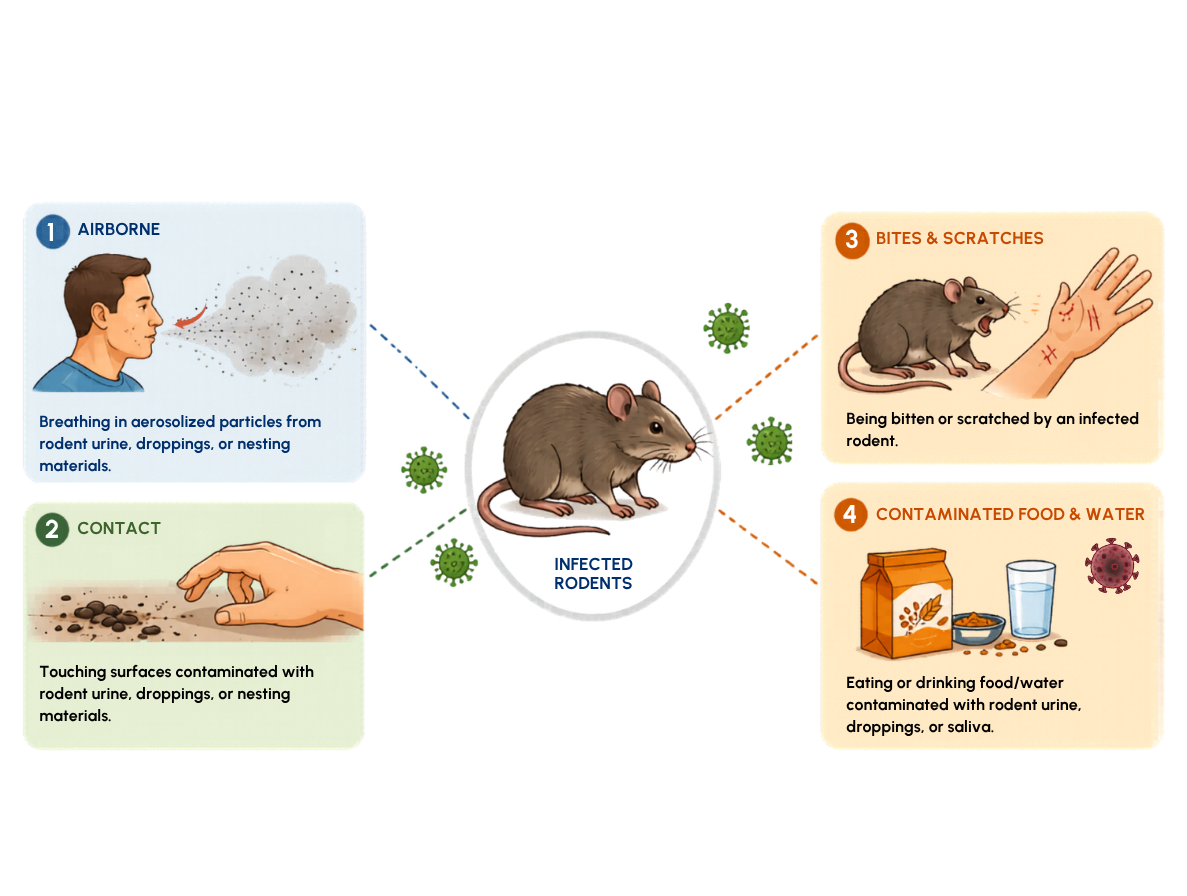
Hantaviruses are rodent-borne viruses that can cause serious disease in humans. Infection usually occurs when people inhale aerosolized particles contaminated with urine, droppings, or saliva from infected rodents. Less commonly, transmission may occur through bites, scratches, or direct contact with contaminated materials.
Recent international attention on hantavirus increased after reports linked to a suspected outbreak investigation aboard the MV Hondius expedition cruise ship in May 2026. The outbreak was linked to Andes virus, a hantavirus strain known for rare person-to-person transmission during close and prolonged contact. Health authorities investigated multiple confirmed and suspected cases among passengers and crew, drawing renewed attention to hantavirus transmission risks and the importance of rapid public health response in confined environments.
What Happens from the Moment of Infection?
The starting point of infection is usually exposure to contaminated rodent materials. After inhalation, the virus enters the body and begins to infect target cells, especially endothelial cells that line blood vessels. Symptoms usually appear within one to eight weeks, depending on the virus type. During the incubation period, the person may feel completely well while the virus begins interacting with host cells and the immune system. Early diagnosis can be difficult because the first symptoms are often non-specific and may resemble influenza, COVID-19, viral pneumonia, leptospirosis, dengue, or sepsis.
As viral replication and immune activation progress, the body begins to produce inflammatory mediators. In some patients, increased vascular permeability may develop, meaning that fluid can leak from blood vessels into surrounding tissues. This process is important in the development of lung involvement in HCPS or kidney involvement in HFRS.
Early hantavirus symptoms are often non-specific and may resemble other viral infections. Common early findings include:
- Fever
- Headache
- Muscle aches
- Fatigue
- Chills
- Nausea or vomiting
- Abdominal pain
- Dizziness
As the disease progresses, symptoms may become more organ-specific. In HCPS, patients may develop cough, shortness of breath, low blood pressure, and respiratory distress. In HFRS, kidney-related findings such as reduced urine output, proteinuria, hematuria, or renal impairment may occur.
Inflammation and Biomarkers
Inflammation plays a major role in hantavirus pathogenesis. Researchers have studied several cytokines and acute-phase proteins to better understand disease severity and progression.
Among these markers, interleukin-6 (IL-6) has attracted particular attention because of its role in endothelial inflammation, immune activation, and vascular leakage. Based on a study on acute Puumala hantavirus infection, higher plasma IL-6 levels were associated with more severe clinical findings, including higher leukocyte counts, greater urinary protein excretion, lower platelet counts, reduced urinary output, and longer hospitalization. In the same study, elevated CRP alone did not reflect disease severity as clearly, suggesting that IL-6 may be a more informative marker of acute disease severity in this context. However, current evidence does not define a universal first-rising marker for all hantavirus infections.
Diagnosis and Clinical Management
CDC indicate that laboratory confirmation may involve serological testing for hantavirus-specific antibodies or molecular detection methods such as RT-PCR during the acute phase. WHO also emphasizes that suspected biological specimens should be handled with appropriate biosafety precautions.
There is currently no licensed specific antiviral treatment or vaccine for hantavirus infection. Management is mainly supportive and focuses on close monitoring and treatment of respiratory, cardiac, or kidney complications. Early intensive care support, when clinically needed, can improve outcomes.
Prevention and Treatment
Prevention mainly depends on reducing contact between people and rodents. Recommended measures include sealing gaps that allow rodents to enter buildings, storing food securely, keeping homes and workplaces clean, avoiding dry sweeping or vacuuming of rodent droppings, dampening contaminated areas before cleaning, and strengthening hand hygiene practices.
There is no specific treatment for hantavirus infection. CDC recommends supportive care to manage symptoms, which may include oxygen therapy, mechanical ventilation, antiviral treatment in selected cases, and dialysis when kidney involvement occurs. Patients with severe symptoms may require admission to an intensive care unit, and in critical cases, intubation may be necessary.
Conclusion
Hantavirus is an important rodent-borne infection that can progress from non-specific early symptoms to severe pulmonary or renal disease. The latest data from the United States show that 890 hantavirus cases were reported in the country between 1993, when surveillance began, and 2023. Because early symptoms may resemble many other infections, exposure history is essential for clinical suspicion. Understanding the route of transmission, symptom timeline, and inflammatory response can support earlier recognition and better public health awareness.
This event has also highlighted the importance of rapid outbreak communication, international coordination, and continued surveillance for emerging zoonotic infections.
References
- World Health Organization. Hantavirus Outbreak Toolbox. Updated May 2026.
- Centers for Disease Control and Prevention. About Hantavirus. 13 May 2024.
- BBC News. Cruise passengers describe life onboard after hantavirus outbreak investigation. BBC News, 2026.
- Outinen TK, et al. The severity of Puumala hantavirus induced nephropathia epidemica can be better evaluated using plasma interleukin-6 than C-reactive protein determinations. BMC Infectious Diseases. 2010.
- Saavedra F, et al. Immune response during hantavirus diseases. 2021.
- World Health Organization. Hantavirus cluster linked to cruise ship travel, Multi-country. Disease Outbreak News. 4 May 2026.