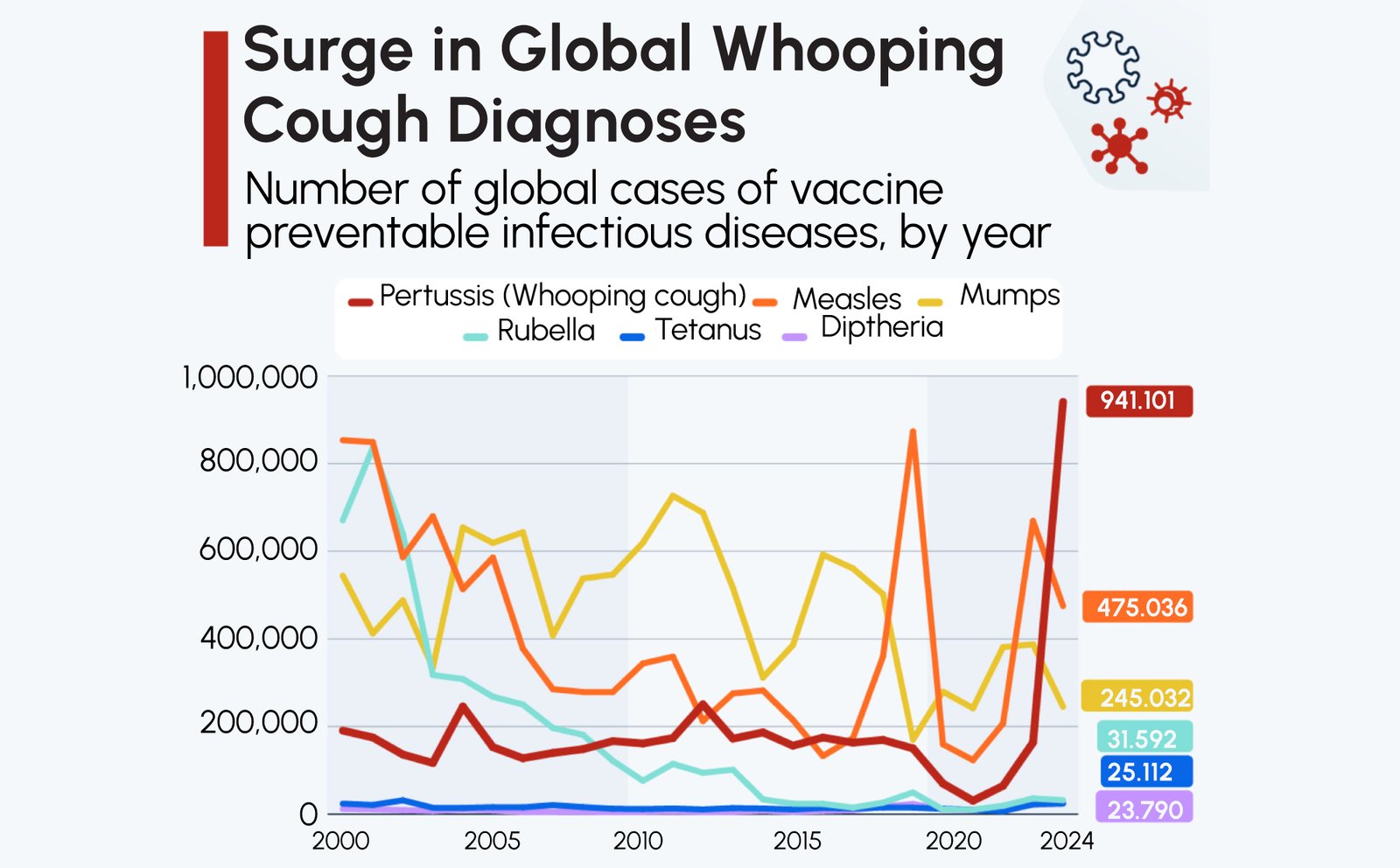
Pertussis, commonly known as whooping cough, is re-emerging globally, with reported cases increasing across multiple regions in 2024–2026. Countries including Australia, the United States, and several regions in Latin America have reported a notable rise in incidence, prompting renewed attention from clinicians and public health systems.
This resurgence reflects a broader shift in respiratory disease dynamics following the COVID-19 pandemic and highlights an ongoing challenge in evaluating patients presenting with persistent or atypical cough.
The Pertussis Resurgence: Epidemiological Evidence From a Post-COVID World
During the COVID-19 pandemic, reported pertussis cases declined significantly, largely due to reduced social interaction, masking, and changes in healthcare utilization. However, this decline reflected reduced transmission rather than elimination.
As public health measures were lifted, pertussis re-emerged in populations with increased susceptibility. Several contributing factors have been observed: reduced natural exposure during pandemic years, particularly in younger populations, waning immunity following acellular pertussis vaccination, disruptions in routine immunization programs in certain regions.
These dynamics have resulted in a broader at-risk population, including not only infants but also adolescents and adults, where presentation may be less typical and more difficult to recognize.
The Clinical and Diagnostic Challenge: Three Stages, Three Diagnostic Windows
Pertussis progresses through three clinical stages, each associated with different symptom patterns and diagnostic considerations. Understanding how these stages evolve is important when interpreting laboratory results and assessing patients with prolonged cough.
The first stage, known as the catarrhal stage, typically lasts 1–2 weeks and presents with mild, non-specific symptoms such as low-grade fever, runny nose, sneezing, and a mild cough. At this stage, the clinical picture closely resembles common respiratory infections, making differentiation difficult. Molecular testing methods such as PCR tend to show the highest sensitivity during this early phase. However, because symptoms are non-specific, pertussis is often not suspected, and testing may not be performed.
The second stage, the paroxysmal stage, can last several weeks and is characterized by episodes of repetitive coughing. Some patients may develop a high-pitched inspiratory sound after coughing, although this is not consistently observed, particularly in adolescents and adults. Infants may present differently, sometimes without typical coughing patterns. As the disease progresses through this stage, the diagnostic yield of PCR declines gradually over time, and culture-based methods have limited sensitivity and longer turnaround times.
The final stage, the convalescent stage, involves gradual symptom improvement, although cough may persist for an extended period. At this stage, molecular and culture-based methods have reduced diagnostic utility, while serological approaches may provide retrospective confirmation.
One of the key challenges in pertussis diagnosis is the mismatch between clinical presentation and optimal testing timing. Early-stage disease, when laboratory detection is most sensitive, often lacks specific clinical features. Later-stage disease, when symptoms become more recognizable, is associated with reduced sensitivity of commonly used diagnostic methods. This contributes to under-recognition, particularly in older age groups where presentation may be atypical.
Differential Diagnosis in the Paroxysmal Cough Patient
In clinical practice, a patient presenting with persistent or paroxysmal cough lasting more than two weeks presents a diagnostic challenge. The differential diagnosis is broad: pertussis, influenza, Streptococcus pyogenes pharyngitis, Mycoplasma pneumoniae infection (walking pneumonia), respiratory syncytial virus (RSV), adenovirus, and other respiratory pathogens.
For patients with high clinical suspicion of pertussis after rapid differential testing is negative, nasopharyngeal PCR for Bordetella pertussis would be ordered. Rapid differential testing supports the clinical evaluation of patients presenting with persistent or paroxysmal cough by providing timely information on common respiratory pathogens. This can help contextualize symptoms and support further diagnostic considerations, including when confirmatory testing such as PCR may be appropriate.
The Vitrosens Bordetella pertussis PCR Solution
Vitrosens offers molecular diagnostic solutions designed to support the detection of respiratory pathogens, including Bordetella pertussis.
The Bordetella pertussis PCR assay is developed to enable reliable detection of target sequences from nasopharyngeal samples, supporting laboratory-based respiratory diagnostics workflows.
Key characteristics of molecular testing within this context include high analytical sensitivity within the appropriate diagnostic window, enabling reliable detection during earlier stages of disease progression. These assays allow for specific identification of Bordetella pertussis genetic targets, supporting targeted laboratory evaluation. In addition, they are compatible with standard molecular laboratory workflows and can be readily integrated into broader respiratory diagnostic panels or testing strategies, contributing to a more comprehensive diagnostic approach.
By combining molecular diagnostics with rapid differential testing, laboratories and healthcare providers can access multiple layers of diagnostic information within a single patient journey.
Conclusion
The pertussis resurgence of 2025-2026 is a reminder that vaccine-preventable diseases remain a persistent threat, particularly when immunity wanes and vaccination coverage gaps emerge. While vaccination is the long-term solution, rapid diagnostics represent an important component of the clinical approach to respiratory infections, supporting earlier identification and a more structured understanding of disease patterns.
In the patient presenting with persistent or paroxysmal cough, rapid differential respiratory testing with quantitative biomarkers provides clinicians with the objective evidence needed to support clinical interpretation, contribute to diagnostic clarity, and help identify patients who may benefit from further confirmatory testing such as PCR. Vitrosens respiratory diagnostic portfolio is designed for these clinical scenarios, delivering rapid, quantitative results at the point of care.
Contact sales@vitrosens.com or visit vitrosens.com to learn how our respiratory differential diagnosis portfolio can strengthen your laboratory’s capacity to manage suspected pertussis cases rapidly and guide evidence-based clinical decisions.
References
- Centers for Disease Control and Prevention. (2025). Pertussis Surveillance and Trends 2025. CDC Press, Atlanta.
- Pan American Health Organization. (2025). Pertussis Outbreaks in the Americas. PAHO Weekly Report.
- Cherry JD. (2012). Epidemic pertussis in 2012, the resurgence of a vaccine-preventable disease. NEJM; 367(9): 785-787.
- Mattoo S, Cherry JD. (2005). Molecular pathogenesis, epidemiology, and clinical manifestations of respiratory infections due to Bordetella pertussis. CMR; 18(2): 326-382.
- Klein NP et al. (2012). Waning protection after fifth dose of acellular pertussis vaccine in children. NEJM; 367(11): 1012-1019.
- Center for Infectious Disease Research and Policy (CIDRAP). (2024). Global Whooping Cough Resurgence Update. University of Minnesota.
- World Health Organization. (2023). Pertussis vaccines: WHO position paper. Wkly Epidemiol Rec; 98(19): 181-196.
- American Academy of Pediatrics. (2024). Pertussis. In: Red Book: Report of the Committee on Infectious Diseases. 34th ed. AAP Press.
- World Health Organization. (2023). Laboratory Manual for the Diagnosis of Whooping Cough Caused by Bordetella pertussis, Bordetella parapertussis, and Bordetella bronchiseptica. WHO Press, Geneva.


