Mycobacterium tuberculosis (TB) is a bacterial infection that primarily affects the lungs but can also affect other parts of the body. TB is a global health concern, with millions of people falling ill and many losing their lives to this disease every year. Early and accurate detection of TB is crucial for effective treatment and prevention of its spread. In this blog, we will explore what Mycobacterium tuberculosis is and how to use a Mycobacterium Tuberculosis (TB) Detection qPCR Kit for diagnosis.

What is Mycobacterium Tuberculosis (TB)?
Mycobacterium tuberculosis, often simply referred to as TB, is a bacterium responsible for causing tuberculosis [1]. TB primarily affects the lungs and is transmitted through the air when an infected person coughs or sneezes, releasing tiny droplets containing the bacteria into the air [1]. When another person inhales these droplets, they can become infected.
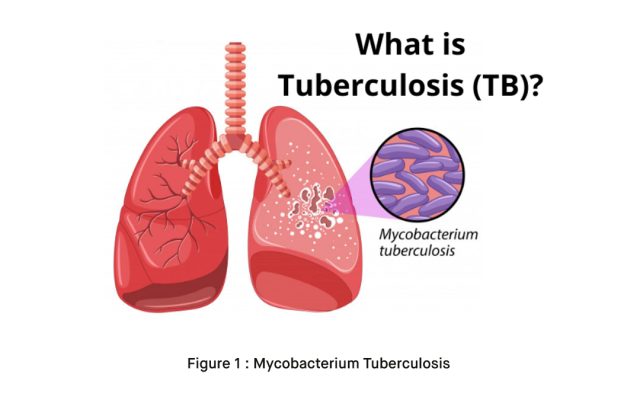
TB can also affect other parts of the body, including the bones, lymph nodes, and even the brain. It can manifest in two forms:
Latent TB Infection: In this form, the bacteria are present in the body but not causing active illness [1]. People with latent TB infection are not contagious and do not show symptoms. However, the bacteria can become active later, leading to active TB disease.
Active TB Disease: This form of TB causes illness and is contagious. Symptoms can include a persistent cough, fever, weight loss, and fatigue. Without proper treatment, active TB can be life-threatening.
Symptoms of Tuberculosis
TB can manifest in different ways, and the symptoms can vary depending on whether it is an active TB infection or a latent TB infection. Here are the common symptoms associated with active TB:
- Persistent Cough
- Fever
- Night Sweats
- Weight Loss
- Fatigue
- Chest Pain
- Shortness of Breath
- Coughing Up Blood

It’s important to note that these symptoms are not exclusive to TB and can be indicative of other respiratory or systemic conditions. Furthermore, in some cases, TB may not cause any symptoms at all, especially in the early stages. This is known as latent TB infection.
If you experience any of these symptoms, especially if they persist for several weeks or are associated with other risk factors such as recent exposure to TB, it is crucial to seek medical evaluation and testing. Early diagnosis and treatment are essential for managing TB effectively and preventing its spread to others. TB is a treatable disease, and with the appropriate medications and care, most people with TB can be cured.
Treatment for Tuberculosis
Treatment for Mycobacterium tuberculosis (TB) involves a course of specific antibiotics that target the TB bacteria. TB treatment is typically divided into two phases: the intensive phase and the continuation phase [2]. The choice of antibiotics and the duration of treatment depend on factors like the type of TB (drug-sensitive or drug-resistant) and the patient’s overall health [2]. Here is an overview of the standard TB treatment:
Intensive Phase:
- First-Line Drugs: The intensive phase begins with a combination of four first-line drugs: Isoniazid (INH), Rifampin (RIF), Pyrazinamide (PZA), Ethambutol (EMB). Patients with confirmed drug-susceptible TB are usually treated with these four drugs for the first two months. This phase is essential to quickly kill the actively dividing TB bacteria [2].
- Continuation Phase: After the intensive phase, the treatment enters the continuation phase, which is designed to eliminate any remaining TB bacteria and prevent relapse. The choice of drugs and duration of the continuation phase depend on several factors:
- For drug-sensitive TB: Isoniazid and Rifampin are continued for an additional 4 to 6 months. This phase can last a total of 6 to 9 months [2].
- For drug-resistant TB: Treatment for drug-resistant TB can be much longer, often extending to 18-24 months. Multiple drugs, including second-line antibiotics, may be used, and the regimen is highly individualized based on drug susceptibility testing [2].
-
Directly Observed Therapy (DOT):
To ensure patients take their medications consistently and correctly, TB treatment is often administered under direct observation, especially during the intensive phase. Healthcare workers or trained community members observe and document the patient taking their medication.
- Monitoring and Adherence: Regular monitoring of treatment progress and side effects is crucial. Patients are encouraged to take their medications as prescribed to prevent the development of drug resistance. Any side effects or issues with treatment should be reported to healthcare providers promptly.
- Drug Resistance Testing: Drug susceptibility testing is performed to determine if the TB bacteria are resistant to any of the standard TB drugs. If drug resistance is detected, a different treatment regimen, including second-line drugs, may be necessary.
- Adjunctive Therapy: In some cases, adjunctive therapies may be used to manage side effects or complications associated with TB, such as anti-nausea medications or liver function monitoring.
- Follow-Up Testing: After completing treatment, patients undergo follow-up testing to ensure the TB infection has been cured. This may involve sputum cultures or other tests to confirm the absence of TB bacteria.
- Preventive Therapy: Individuals with latent TB infection (LTBI) may receive a recommendation for preventive therapy with a single drug like isoniazid to reduce their risk of developing active TB disease.
It’s crucial to complete the entire course of treatment, even if symptoms improve before finishing the prescribed medication. Stopping treatment prematurely can lead to treatment failure, relapse, or the development of drug-resistant TB.
TB treatment should be managed by healthcare professionals with expertise in tuberculosis care to ensure the best outcomes. Patient education, adherence support, and close monitoring are essential components of successful TB treatment.
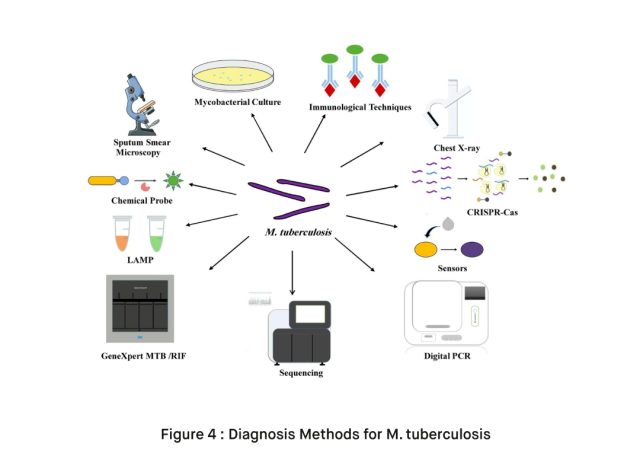
Diagnosis Methods of TB
Diagnosing tuberculosis (TB) involves a combination of clinical evaluation, medical history, and various diagnostic tests to confirm the presence of Mycobacterium tuberculosis, the bacterium responsible for TB. Accurate and timely diagnosis is essential for effective treatment and prevention of the spread of the disease. Here are some common methods used for diagnosing TB:
- Medical History and Clinical Evaluation:
- A thorough medical history and clinical examination are essential initial steps in diagnosing TB. Healthcare providers will ask about symptoms, risk factors (such as recent exposure to TB), and any relevant medical conditions.
- Tuberculin Skin Test (TST) or Mantoux Test:
- The TST is a common screening test for TB infection. A small amount of purified protein derivative (PPD), a substance derived from the TB bacteria, is injected just beneath the skin [3] . After 48-72 hours, the healthcare provider checks for a raised, red bump at the injection site. The size of the bump indicates the presence of a TB infection. However, this test cannot distinguish between latent TB infection (LTBI) and active TB disease.
- Interferon-Gamma Release Assays (IGRAs):
- IGRAs are blood tests that measure the release of interferon-gamma (a substance produced by the immune system) in response to TB-specific antigens [3]. These tests can help differentiate between LTBI and active TB disease.
- Chest X-ray:
- Chest X-rays are a valuable tool for diagnosing pulmonary TB. They can reveal abnormalities in the lungs, such as characteristic patterns of TB infection, cavities, or lung damage. However, a chest X-ray alone cannot confirm the presence of TB; additional tests are needed.
-
Sputum Smear Microscopy:
- This test involves examining sputum (mucus coughed up from the lungs) under a microscope to check for the presence of acid-fast bacilli (AFB), which are characteristic of Mycobacterium tuberculosis [3]. It is a rapid but less sensitive method, often used for initial screening.
- Sputum Culture:
- Sputum samples can be cultured in a laboratory to grow Mycobacterium tuberculosis bacteria. This is a more definitive diagnostic method that confirms the presence of TB and allows for drug susceptibility testing to determine appropriate treatment.
- Nucleic Acid Amplification Tests (NAATs):
- NAATs, such as MTB/RIF assay, detect TB-specific DNA or RNA in sputum or other clinical samples. They are highly sensitive and can also identify rifampin resistance, a common marker for multidrug-resistant TB.
- Biopsy and Histopathology:
- In cases of extrapulmonary TB (TB affecting organs other than the lungs), a tissue biopsy may be necessary. The biopsy sample is examined under a microscope for the presence of TB bacteria.
- Bronchoscopy:
- For individuals unable to produce sputum or when other tests are inconclusive, a bronchoscopy may be performed. This involves passing a flexible tube through the throat and into the lungs to collect samples for testing.
- Molecular Tests:
- Polymerase chain reaction (PCR) and other molecular tests can detect TB DNA or RNA in clinical samples, offering a rapid and sensitive diagnosis.
The choice of diagnostic method depends on several factors, including the patient’s clinical presentation, risk factors, and the availability of resources. In cases where TB is suspected, it is essential to consult with a healthcare provider who can determine the most appropriate diagnostic approach to confirm or rule out TB infection. Early diagnosis is crucial for prompt treatment and preventing the spread of TB.
Detecting TB with a TB Detection PCR Kit
Polymerase Chain Reaction (PCR) is a molecular biology technique used to amplify specific DNA sequences. A TB Detection PCR Kit utilizes this technology to identify the presence of Mycobacterium tuberculosis DNA in a patient’s sample. Here’s how to use a TB Detection PCR Kit:
Sample Collection: Collect a sample from the patient. For pulmonary TB, this is often sputum (mucus coughed up from the lungs). Other samples, such as blood or urine, can be used for extrapulmonary TB.
Sample Preparation: Process the collected sample to extract DNA. This step may involve breaking down cell walls and proteins to isolate the genetic material.
PCR Reaction: Set up a PCR reaction using the extracted DNA. The PCR mixture contains specific primers that target Mycobacterium tuberculosis DNA and enzymes that replicate the DNA segments.
Amplification: Run the PCR machine through a series of cycles that heat and cool the reaction mixture. This process exponentially multiplies the target DNA if Mycobacterium tuberculosis is present.
Detection: The PCR machine monitors the reaction in real-time. If Mycobacterium tuberculosis DNA is present in the sample, it will produce a fluorescent signal, indicating a positive result.
Analysis: Analyze the results. A positive result indicates the presence of Mycobacterium tuberculosis DNA, suggesting an active infection. A negative result does not rule out TB, especially in cases of extrapulmonary TB, as the bacteria may not always be present in the collected sample.
Interpretation and Diagnosis: The results are interpreted by a healthcare professional, who will use them to diagnose TB and determine the appropriate treatment.
What is the Most Effective And Common Mycobacterium Tuberculosis Detection qPCR Kit?
The CHAINFOR™ Mycobacterium Tuberculosis Detection qPCR Kit is designed for in vitro qualitative diagnosis of various Mycobacterium tuberculosis complex strains, including M. tuberculosis, M. bovis, M. africanum, M. microti, M. caprae, M. canetti, and the vaccine strain BCG. This kit is intended for use with sputum and bronchoalveolar lavage samples.
Key features of the CHAINFOR Mycobacterium Tuberculosis Detection qPCR Kit include:
- Rapid RT-PCR test: It enables Real-Time PCR for the detection of Mycobacterium tuberculosis nucleic acids.
- Fast results: The kit allows for the completion of RT-qPCR testing in just 50 minutes.
- Comprehensive: It can detect 7 different Mycobacterium genotypes, providing valuable information for diagnosis.
This kit appears to offer a quick and efficient method for identifying various Mycobacterium tuberculosis complex strains in respiratory samples, aiding in the timely diagnosis and management of tuberculosis.

REFERENCES
[1] Koch, A., & Mizrahi, V. (2018). Mycobacterium tuberculosis. Trends in microbiology, 26(6), 555-556.
[2] AlMatar, M., AlMandeal, H., Var, I., Kayar, B., & Köksal, F. (2017). New drugs for the treatment of Mycobacterium tuberculosis infection. Biomedicine & Pharmacotherapy, 91, 546-558.
[3] Al-Zamel, F. A. (2009). Detection and diagnosis of Mycobacterium tuberculosis. Expert review of anti-infective therapy, 7(9), 1099-1108.


