What are Influenza Type A Flu and Type B Flu?

Influenza, or flu, is a common and highly infectious respiratory disease caused by various types of influenza viruses. Influenza viruses are single-stranded segmented RNA viruses of the family Orthomyxoviridae, which primarily spread via droplets or respiratory secretions of infected people. Influenza is quite common all around the world, especially in fall and winter. In fact, according to World Health Organization (WHO), influenza affects 5 – 10% of adults and 20 – 30% of children every year.
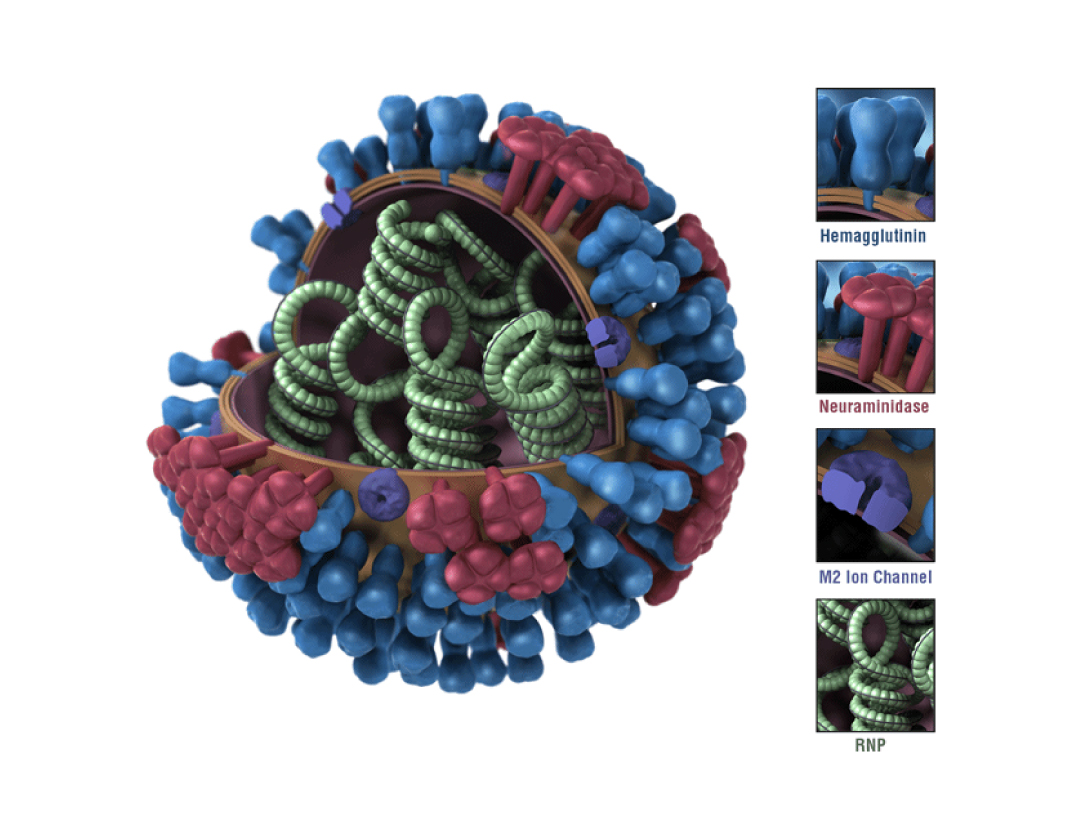
Similar to many other RNA genome viruses, influenza virus undergoes rapid, frequent, and continuous mutations through the combination and rearrangement of genetic material. There are currently four types of influenza viruses, which are influenza A, B, C, and D. Influenza A and B are recognized as the only types of the virus to cause human disease of any concern, as Influenza C has not been associated with severe symptoms or epidemics in humans and influenza D has been found to only affect cattle and swine populations. Read along to find out more about influenza A and B, along with their symptoms, diagnosis, and treatment.
What are the differences between Influenza Type A and Influenza Type B?
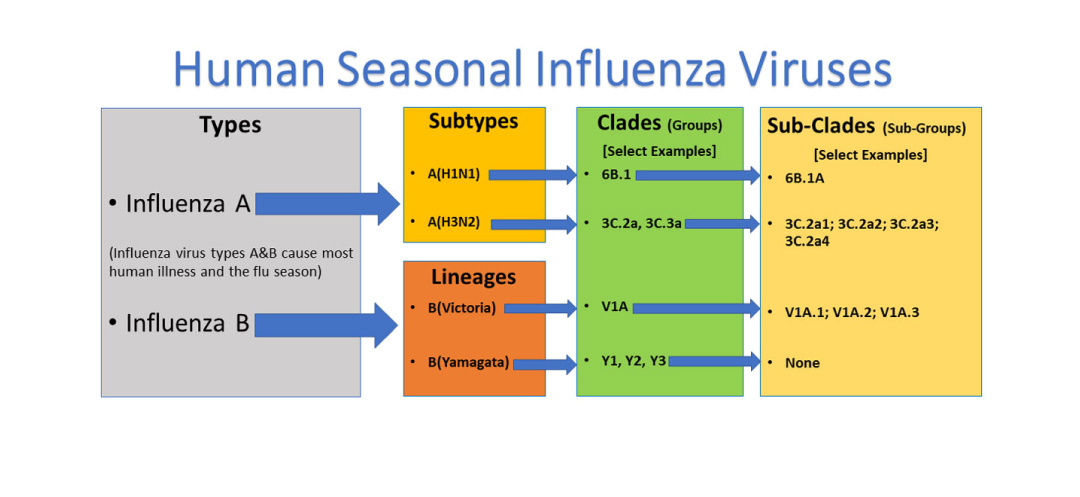
Influenza A has been found to have a significantly higher mutation rate than influenza B. In fact, several studies have demonstrated that most genes in influenza A viruses mutate two to three times faster than the corresponding genes in influenza B viruses. Accordingly, Influenza A is further classified into various subtypes depending on the combination of their envelope glycoproteins haemagglutinin (H) and neuraminidase (N). Given that there are 18 known haemagglutinin (H) subtypes and 11 known neuraminidase (N) subtypes, many different combinations of these proteins are possible. Many of the known subtype combinations have been discovered in birds and bats, and influenza A viruses have been known to circulate in non-human animals including wild water birds, domestic poultry, swine, horses, dogs, bats, and less commonly in cats and seals. However, influenza A subtypes circulating among humans have been limited to A(H1N1), A(H2N2), and A(H3N2) for the last century. Among these, A(H1N1) and A(H3N2) are currently most common subtypes circulating in people. Unlike influenza A, influenza B is only classified into specific viral lineages and strains. Based on viral lineage, influenza B viruses have been classified into two lineages, Victoria and Yamagata. Again, whereas influenza A commonly infects various animal species and groups, influenza B is known to only affect humans, and to a lesser extent, seals.

Moreover, likely due to its high mutation rate and extensive host range of the virus, influenza A is capable of causing pandemics and large epidemics. Indeed, Spanish Flu (1918), Asian Flu (1957), Hong Kong Flu (1968), Bird Flu (2004), and Swine Flu (2009) have all been caused by various subtypes of influenza A. Even though it has been responsible for epidemics, influenza B has never been known to cause a pandemic. Influenza A is also significantly more prevalent than influenza B. In fact, according to a study by Nyirenda et al. (2016), influenza A infections are responsible for around 75 percent of all confirmed seasonal influenza infections.
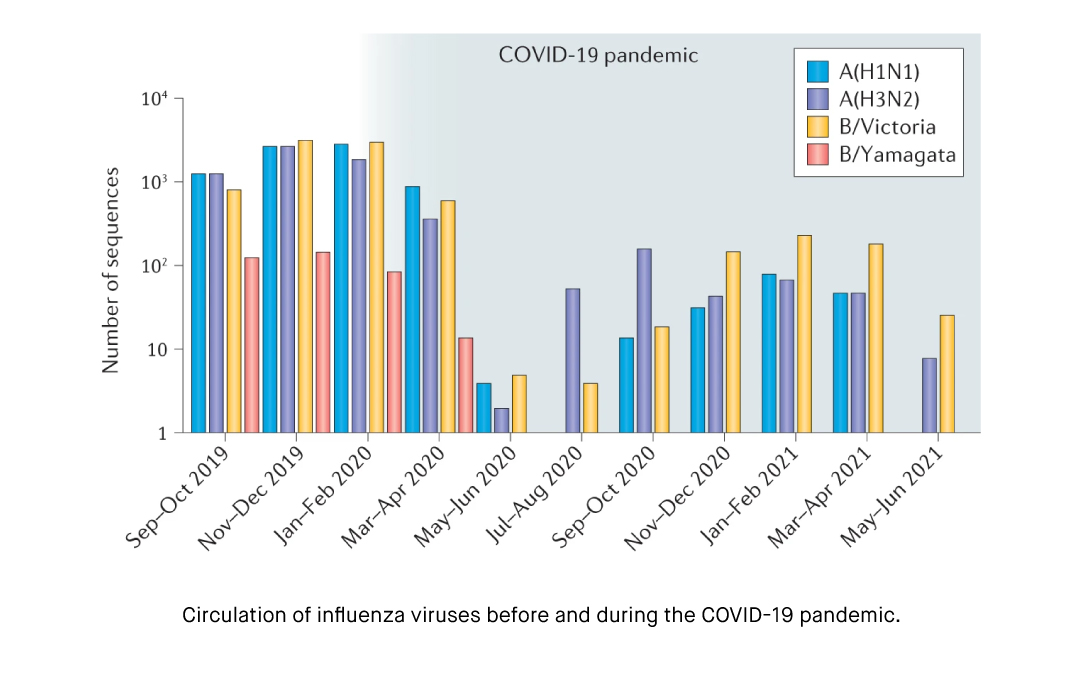
In terms of disease severity, there is evidence to suggest that infections with some subtypes of influenza A may cause more severe disease than influenza B and other subtypes of influenza A. For instance, Wie et al. (2013) have found that rates of hospitalization and length of hospital stay were higher in patients infected with subtype A(H3N2) than those infected with influenza B. Moreover, according to data by the Centers for Disease Control and Prevention (CDC) covering the 2017-2018 flu season, influenza A accounted for 84.1 % of positive samples and 86.4 % of hospitalizations overall. Still, several studies have linked the higher rates of hospitalization associated with influenza A to its prevalence rather than its clinical characteristics. Indeed, studies such as Su et al. (2014) and Mosnier (2015) have found similar or comparable clinical features between patients infected with influenza A and B virus in outpatient settings, and some studies have shown substantial and even higher rates of mortality linked to pediatric influenza B infections relative to influenza A infections (Paddock et al., 2012; Tran et al., 2016).
What are the signs and symptoms of Influenza Type A and Influenza Type B?

Although some studies have shown that certain symptoms might be more common in influenza A or influenza B, signs and symptoms of influenza A and influenza B are largely similar. Symptoms of uncomplicated infection with either type of influenza typically include fever, cough, sore throat, runny or stuffy nose, sore throat, fatigue, headaches, and myalgia. Some people, especially children, can also experience vomiting or diarrhea. For most healthy people, influenza symptoms typically resolve within a week. However, some people, including those who are older than 65, young children, immunocompromised people, people with certain chronic illnesses, pregnant women, and people with a body mass index (BMI) of 40 or more are at increased risk of developing more severe and prolonged symptoms or complications. Complications associated with influenza include asthma flare-ups, pneumonia, bronchitis, myocarditis, encephalitis, heart problems, and multi-organ failure.
How are Influenza Type A and Influenza Type B diagnosed?

Various methods of testing are available for the diagnosis of influenza, including rapid antigen testing, rapid molecular testing, and laboratory testing. Rapid antigen testing is commonly used in the diagnosis of influenza. Rapid antigen tests can detect and differentiate infections with influenza A and influenza B, and deliver results in 15 to 20 minutes. Further, as these tests do not require laboratory equipment or highly trained personnel, rapid antigen tests can be performed at the point-of-care, and some have even been designed for self-administration. More recently, combined rapid antigen tests, such as our RapidFor™ SARS-CoV-2 & FLU A/B Combo Antigen Test Kit and RapidFor™ FLU A/B Rapid Antigen Test Kit have enabled the simultaneous differential detection of infections such as influenza, COVID-19, and RSV which may have similar symptoms. Using only a single specimen, these tests can quickly determine the pathogen responsible for the infection, which facilitates timely and accurate treatment for infections with similar symptoms. However, due to their higher sensitivity and specificity, molecular testing methods such as RT-PCR are recommended for use in hospitalized patients.
How is influenza treated?
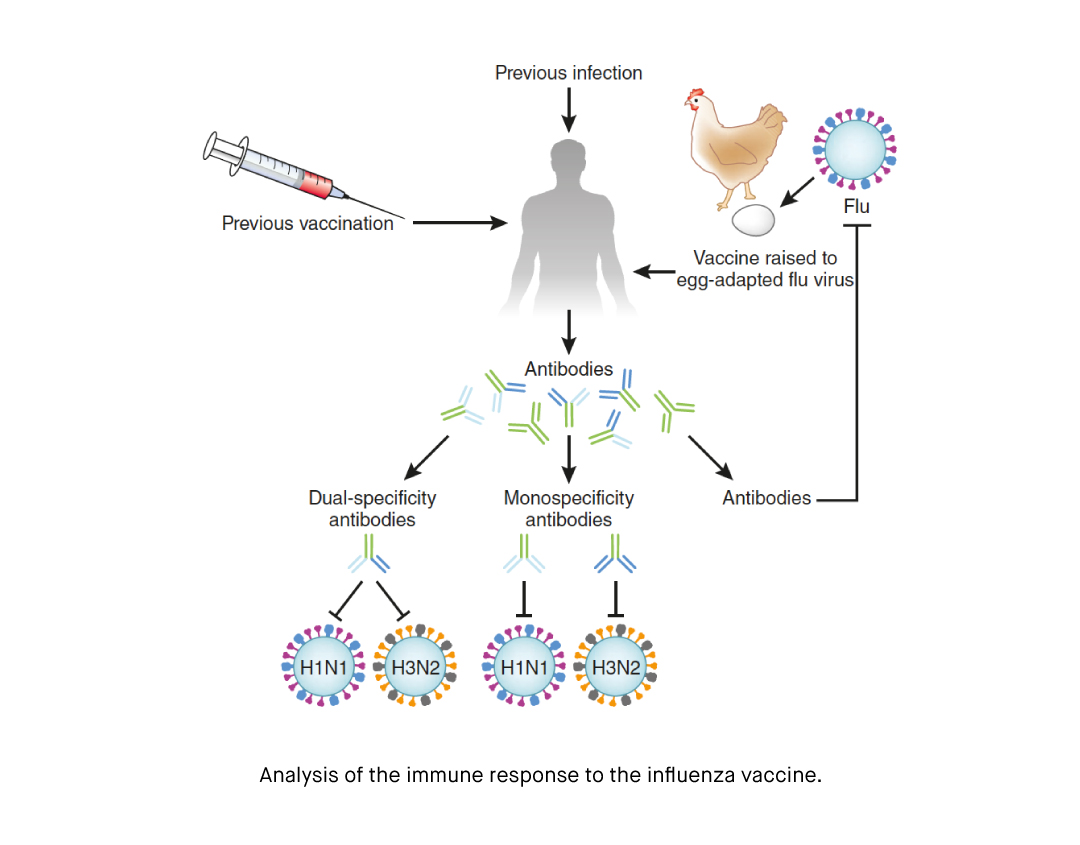
Treatment of influenza typically aims to relieve the symptoms until the immune system naturally fights it off. Thus, resting, eating a healthy diet, and staying hydrated can help you recover more quickly. Over-the-counter medications can also be taken to relieve the symptoms of influenza. In some cases, antiviral medications such as zanamivir, peramivir, and oseltamivir can be prescribed to treat or prevent influenza infections. Influenza vaccine, which covers both influenza A and B, are also available. New versions of the vaccine are developed every year according to the changes of the virus and estimations regarding the upcoming flu season. Although the effectiveness of the influenza vaccines is variable, most vaccines offer moderate to high protection. According to CDC, in flu season where vaccine viruses are similar to circulating viruses, the influenza vaccine has been demonstrated to reduce the risk of having to go to to the doctor with flu by 40-60%. several studies have also shown that influenza vaccination can reduce the risk of severe disease, hospitalization, and complications associated with influenza.

