Antimicrobial Resistance (AMR) is an escalating global health emergency that poses a serious threat to health systems and economies. The recently published report by the World Health Organization (WHO) sheds light on the potential catastrophic consequences of AMR in the Western Pacific Region, home to 37 nations, including Australia, Japan, and Singapore. The findings project a grim scenario, indicating that between 2020 and 2030, over 5.2 million lives could be lost to drug-resistant bacterial infections.

Causes of Antimicrobial Resistance
The origins of AMR can be traced to the misuse and overuse of antimicrobial agents. Antibiotics, which were once hailed as miracle drugs, are now facing resistance as bacteria, viruses, fungi, and parasites adapt over time. Factors contributing to AMR include:
- Inappropriate Antibiotic Use: Overprescription and misuse of antibiotics, often in response to viral infections where antibiotics are ineffective, contribute to the development of resistance.
- Agricultural Practices: Widespread use of antibiotics in agriculture for livestock growth promotion and disease prevention contributes to the spread of resistance.

Why antibiotic resistance develops and spreads. - Incomplete Treatment Courses: Failure to complete prescribed antibiotic courses allows surviving bacteria to develop resistance.
- Lack of New Antibiotics: The slow pace of developing new antibiotics exacerbates the problem, as existing drugs become less effective.
Symptoms of Antimicrobial Resistance Infections
The symptoms of AMR infections are similar to those of non-resistant infections, making diagnosis challenging based solely on clinical presentation. Common symptoms may include:
- Fever
- Fatigue
- Pain or discomfort
- Coughing or respiratory symptoms
- Urinary symptoms
Unveiling the Silent Pandemic
AMR operates quietly but significantly, leading to infections that are increasingly challenging to treat. In the Western Pacific Region, the death toll from AMR is anticipated to surpass that of HIV/AIDS and tuberculosis combined, marking it as a ‘silent pandemic.’ The superbugs responsible for this grim projection are primarily MRSA (methicillin-resistant Staphylococcus aureus) and E. coli, which are expected to account for more than 80% of the projected deaths.
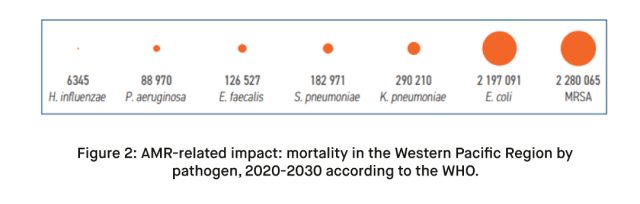
Economic Fallout
The impact of AMR extends beyond human lives, manifesting in substantial economic repercussions. The estimated economic cost of AMR in the Western Pacific Region is a staggering £120 billion. This cost encompasses lost productivity and additional healthcare expenses associated with prolonged hospitalizations due to drug-resistant infections. The economic burden emphasizes the urgency for governments to address AMR as a critical policy and financial priority.

A Global Health Challenge
AMR is not confined to a specific region; it is a global challenge requiring concerted efforts to mitigate its impact. Globally, AMR caused more deaths in 2020 than tuberculosis and HIV/AIDS. The increasing rate of antibiotic resistance, coupled with a dearth of new antibiotics in development, raises concerns about our ability to effectively combat bacterial infections in the future.
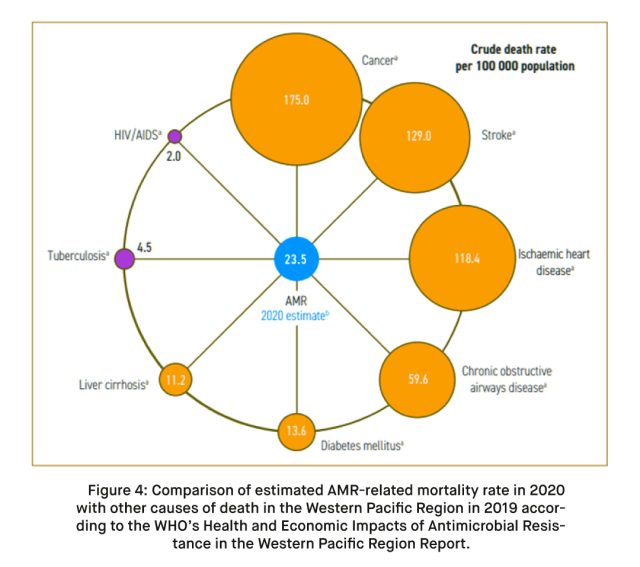
Risk Groups
Certain populations are more vulnerable to AMR infections, including:
- Immunocompromised Individuals: Those with weakened immune systems, such as cancer patients undergoing chemotherapy or organ transplant recipients, are at higher risk.
- Elderly Individuals: Aging is associated with a natural decline in immune function, making the elderly more susceptible.
- Children: The immune systems of children are still developing, making them more prone to infections.
- Patients in Healthcare Settings: Those undergoing medical procedures, surgeries, or prolonged hospital stays face an increased risk of AMR infections.
Urgent Action and Investments
The WHO report serves as a call to action for governments and policymakers to prioritize interventions that address AMR. Investments made now to tackle the ‘silent pandemic’ are considered essential for averting a future health crisis and safeguarding economies. The estimated cost of resistance in the Western Pacific Region underscores the need for substantial investments, which, if made promptly, can result in considerable savings in future healthcare costs.

Diagnosis Methods
Accurate and timely diagnosis of AMR infections is crucial for effective treatment. Diagnosis methods include:
- Laboratory Cultures: Identifying the specific microorganism causing the infection and testing its susceptibility to various antibiotics.
- Molecular Techniques: DNA-based methods to detect resistance genes and predict the resistance profile of the infecting microorganism.
- Biomarker Detection: Identifying specific biomarkers associated with drug resistance.
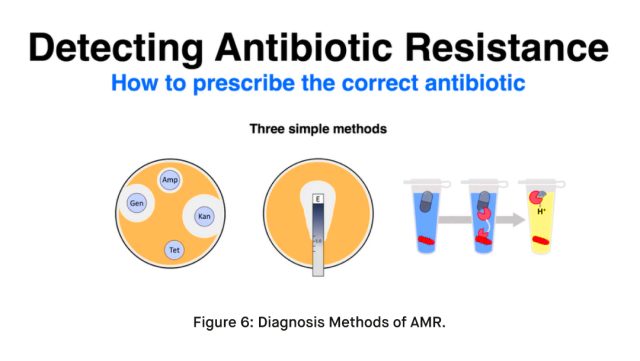
Diagnosis Methods of AMR.
Environmental Concerns and Cross-Cutting Impact
AMR is not only a healthcare issue but also an environmental concern. Traces of antibiotics found in sewage and wastewater treatment plants in Southeast Asia and the Western Pacific raise alarms about potential hotspots for the emergence of drug-resistant infections. The cross-cutting impact of AMR extends to maternal and child health, infectious disease management, cancer therapy, surgical interventions, and health security.
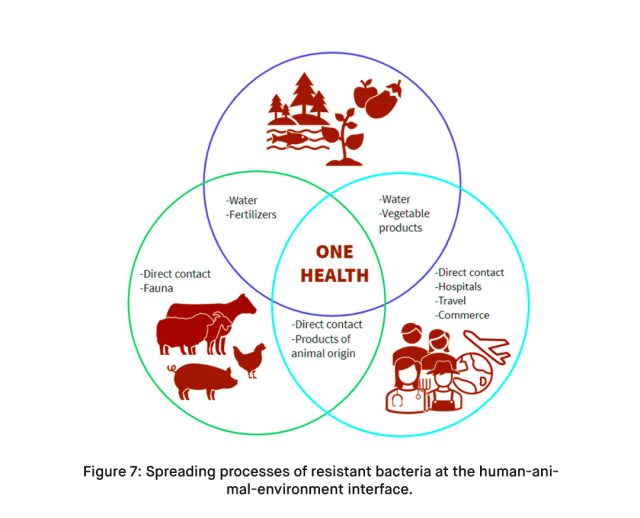
Treatment Strategies
Managing AMR requires a multifaceted approach:
- Antimicrobial Stewardship: Implementing policies to ensure appropriate use of antimicrobial agents in healthcare settings.
- Development of New Antibiotics: Investing in research and development to create new drugs that can combat resistant strains.

ematic representation of newer approaches to tackle AMR Pathogen: These are the set of approaches that are currently under research for efficient treatment of AMR pathogen based infection and its spread. - Combination Therapies: Using a combination of antimicrobial agents to enhance effectiveness and reduce the risk of resistance.
- Public Health Education: Raising awareness about responsible antibiotic use, both in medical and agricultural settings.
Addressing AMR requires a comprehensive and collaborative approach. It involves strengthening surveillance systems, reducing inappropriate antimicrobial use, and investing in research and development for new medicines, vaccines, and diagnostic tools. The WHO’s regional assessment serves as a crucial step in understanding and mitigating the impact of AMR, emphasizing the need for immediate and sustained action to avert a future health crisis.
As the ‘silent pandemic’ continues to unfold, global cooperation and investments in combating antimicrobial resistance become paramount. The time to act is now, as the consequences of inaction are not only measured in economic terms but, more importantly, in human lives lost to preventable and treatable infections.
REFERENCES
- World Health Organization. Essential Medicines and Health Technologies (EMT), WHO Western Pacific. Health and Economic Impacts of Antimicrobial Resistance in the Western Pacific Region, 2020–2030. WHO Regional Office for the Western Pacific; 2023.
- Murray CJ, Ikuta KS, Sharara F, Swetschinski L, Aguilar GR, Gray A, et al. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. The Lancet. 2022.
- World Health Organization. Regional Office for the Western Pacific. Framework for accelerating action to fight antimicrobial resistance in the Western Pacific Region. WHO Regional Office for the Western Pacific; 2020.
- Bhandari, V., & Suresh, A. (2022). Next-Generation approaches needed to tackle antimicrobial resistance for the development of novel therapies against the deadly pathogens. Frontiers in Pharmacology, 13, 838092.
- World Bank. Drug-resistant infections: a threat to our economic future. Washington D.C.: World Bank; 2017.
- World Health Organization (WHO). Antimicrobial Resistance and Primary Healthcare. 2018.


